Adolescent Male Mental Health

In 2021, a study published in The Journal of Adolescence revealed a startling statistic: only 13.2% of adolescent males with a diagnosable mental health condition accessed professional services. This figure, drawn from a comprehensive analysis of Australian youth, underscores a pervasive issue—young men are not only less likely to seek help but are also more likely to mask their struggles behind behaviors often misinterpreted as defiance or apathy.
The roots of this phenomenon extend deep into societal constructs. Dominant masculine ideals—stoicism, emotional control, and invulnerability—discourage open acknowledgment of mental health challenges. Dr. Simon Rice, a leading researcher in adolescent male mental health at Orygen, notes that these cultural expectations "create a barrier to recognizing distress, let alone seeking support." Compounding this is the fact that male adolescents frequently exhibit atypical symptoms of mental illness, such as aggression or substance misuse, which clinicians may overlook or misdiagnose.
The implications are profound. Untreated mental health conditions in adolescence often persist into adulthood, contributing to higher rates of substance dependency, interpersonal violence, and even suicide. According to the Australian Institute of Health and Welfare, suicide remains the leading cause of death among males aged 15–24, a grim testament to the urgency of addressing this crisis.
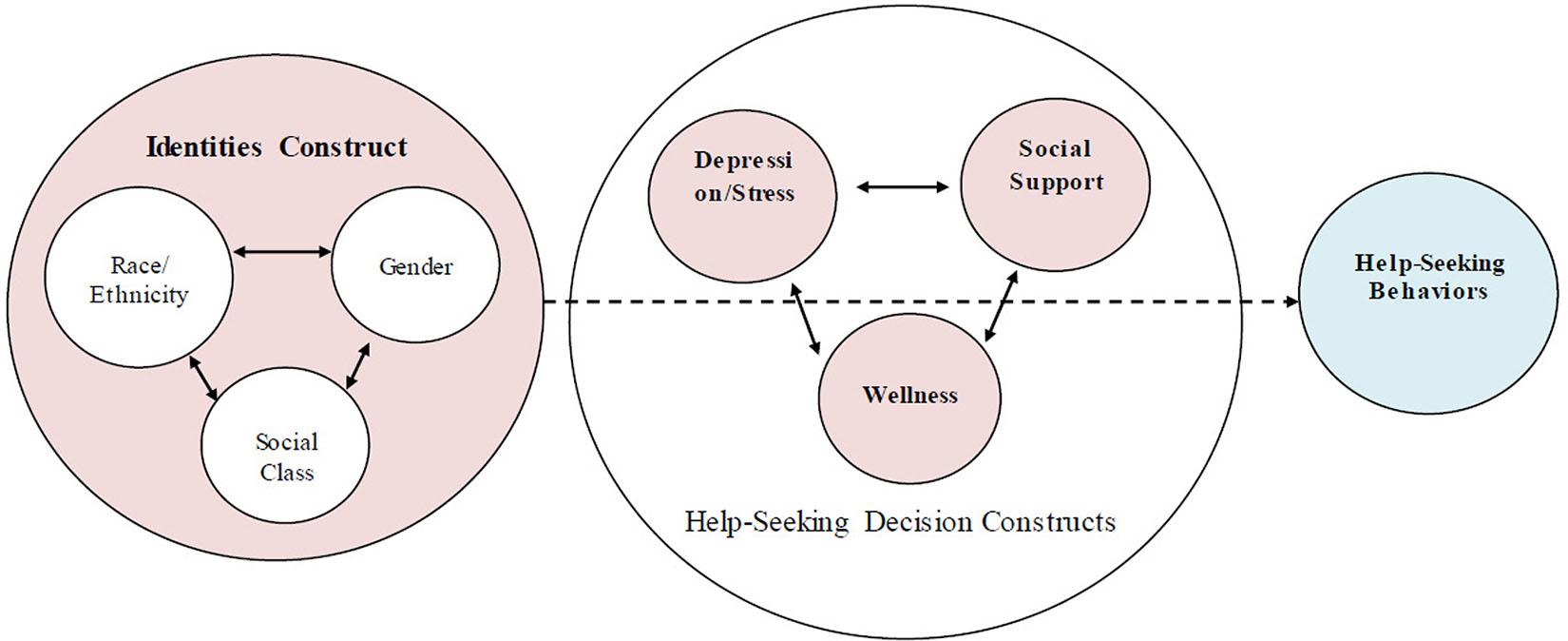
Defining Mental Health in Adolescence
Adolescent mental health is intricately tied to the interplay of neurodevelopmental changes and sociocultural expectations [5], particularly for males. During this critical period [1], [2], the brain undergoes significant remodeling, especially in the prefrontal cortex, which governs decision-making and emotional [3], [4] regulation. This biological evolution coincides with heightened societal pressures to conform to traditional masculine norms, often discouraging emotional expression and vulnerability.
A key challenge lies in the diagnostic frameworks traditionally employed. These frameworks often prioritize internalized symptoms, such as sadness or withdrawal, while externalized behaviors—common among adolescent males—are frequently misinterpreted. For instance, irritability, impulsivity, or risk-taking may be dismissed as typical teenage behavior rather than potential indicators of underlying distress. This diagnostic gap is compounded by the stigma surrounding mental health, which further deters young males from seeking help.
"The nuanced presentation of mental health issues in adolescent males demands a paradigm shift in how we assess and address their needs,"
— Dr. Timothy R. Rice, Adolescent Mental Health Specialist
Emerging approaches advocate for gender-sensitive assessment tools that integrate behavioral, emotional, and contextual factors. For example, school-based interventions in Norway have demonstrated success by normalizing discussions around mental health and training educators to recognize nontraditional symptoms. These programs highlight the importance of creating environments where adolescent males feel safe to express vulnerability without fear of judgment.
Ultimately, redefining mental health in adolescence requires a multifaceted approach that bridges biological, psychological, and social dimensions, ensuring that interventions are both inclusive and responsive to the unique challenges faced by this demographic.
Gender-Specific Risk Factors
The intersection of neurodevelopmental vulnerabilities and societal constructs uniquely shapes the mental health risks faced by adolescent males [9]. One critical factor is the heightened prevalence of externalizing behaviors, such as aggression or substance misuse, which often mask underlying psychological distress. These behaviors, while frequently dismissed as normative adolescent rebellion, are indicative of deeper issues when viewed through a gender-sensitive lens.
A significant challenge lies in the diagnostic frameworks that prioritize internalized symptoms, such as sadness or withdrawal, over externalized manifestations [7], [8]. This misalignment is particularly problematic given that male adolescents are more likely to exhibit distress through actions rather than verbal expressions. For instance, studies utilizing the Strengths and Difficulties Questionnaire (SDQ) have demonstrated that boys with low family cohesion or parental depressive symptoms are disproportionately at risk for behavioral disorders, underscoring the need for contextually aware assessments.
Moreover, the interplay between societal expectations and neurobiological development exacerbates these risks. The delayed maturation of the male prefrontal cortex, responsible for impulse control and emotional regulation [1], [6], creates a window of vulnerability during adolescence. This developmental lag, compounded by cultural norms that valorize stoicism and emotional suppression, fosters maladaptive coping mechanisms.
"Without addressing the societal and biological underpinnings of male adolescent behavior, we risk perpetuating cycles of misdiagnosis and inadequate care."
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
To mitigate these risks, integrating gender-specific diagnostic tools and early intervention strategies is imperative. Tailored approaches that account for both behavioral and contextual factors can bridge the gap between clinical understanding and real-world application, ultimately fostering more effective mental health outcomes.
Prevalence and Types of Mental Health Conditions
Adolescent males exhibit distinct patterns in the prevalence and manifestation of mental health conditions, shaped by both biological and sociocultural factors. Anxiety disorders, for instance, affect approximately 26.1% of male adolescents in the United States, a figure that underscores the need for targeted interventions. However, unlike their female counterparts, young males are more likely to externalize distress through behaviors such as aggression or substance misuse, complicating accurate diagnosis and treatment.
Attention deficit-hyperactivity disorder (ADHD) is another condition disproportionately affecting this demographic [10], [11], with prevalence rates ranging from 7.5% to 9.4%. Untreated ADHD often coexists with oppositional defiant disorder or conduct disorder, leading to cascading challenges such as academic failure, family conflict, and increased risk-taking behaviors, including reckless driving. These comorbidities highlight the necessity of comprehensive, multi-faceted treatment approaches that address both primary and secondary conditions.
A particularly alarming statistic is the suicide rate among adolescent males [12], which is three times higher than that of females in the same age group. This disparity is not merely a reflection of higher lethality in methods but also of underlying factors such as untreated depression, often masked by irritability or agitation. Such presentations are frequently misinterpreted [8], [1], further delaying critical interventions.
These findings emphasize the importance of gender-sensitive diagnostic frameworks that account for the unique ways adolescent males experience and express mental health challenges. By integrating behavioral, emotional, and contextual factors, clinicians can better address the complex interplay of conditions affecting this vulnerable population.
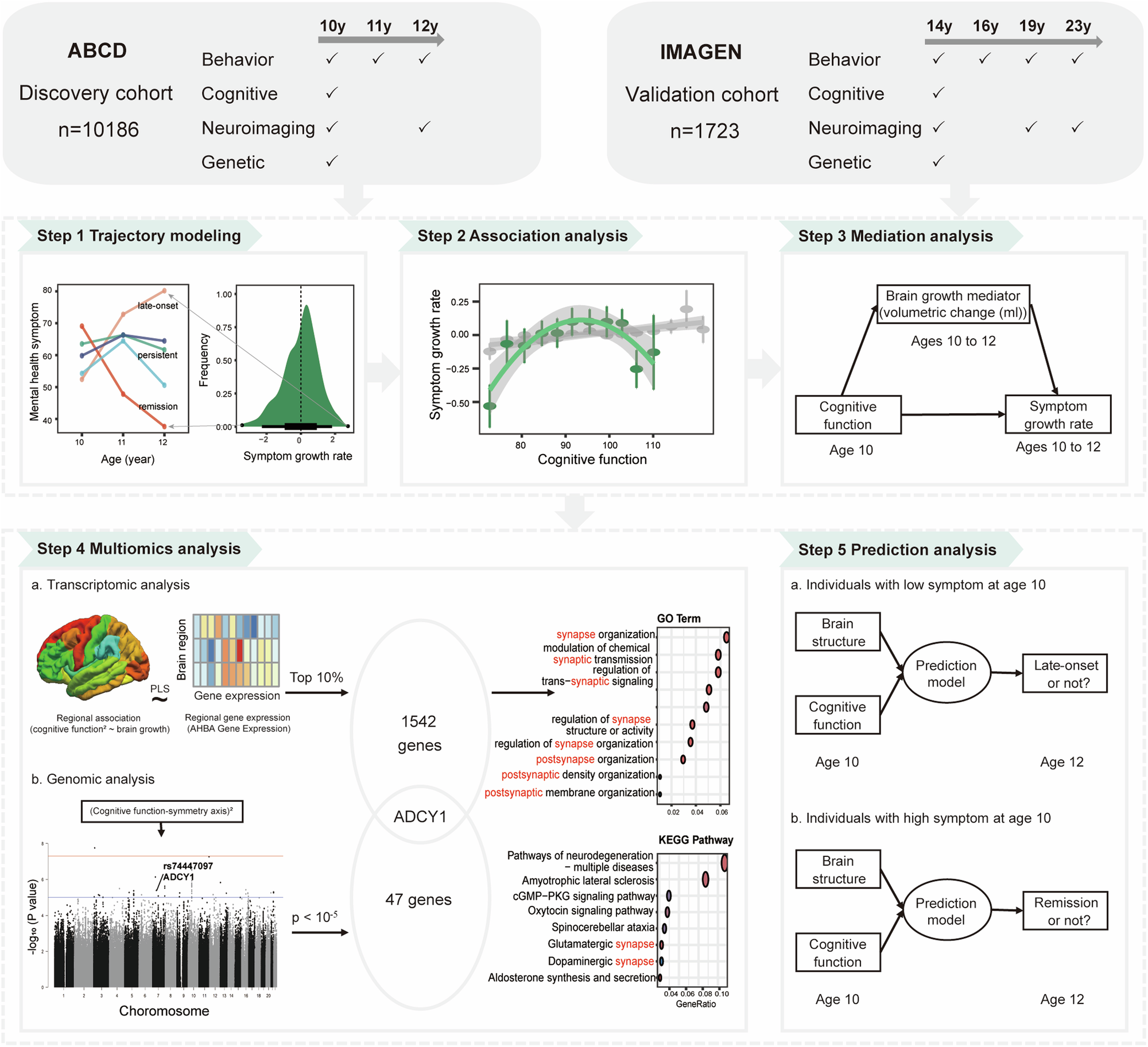
Common Disorders in Adolescent Males
The diagnostic complexity of Attention-Deficit/Hyperactivity [14] Disorder (ADHD [7], [1]) in adolescent males underscores a critical intersection of neurodevelopmental and sociocultural factors. ADHD, characterized by persistent patterns of inattention, hyperactivity, and impulsivity, is diagnosed in 13.0% of male adolescents, a rate significantly higher than their female counterparts [13], [8]. This disparity is partially attributed to gendered expectations, where externalizing behaviors in boys are often normalized or misinterpreted as defiance rather than symptoms of a clinical condition.
A key challenge lies in the overreliance on traditional diagnostic criteria, which inadequately address the nuanced presentations of ADHD in males. For instance, impulsivity and hyperactivity may manifest as risk-taking or disruptive classroom behavior, leading to disciplinary actions rather than therapeutic interventions. Comparative studies reveal that while boys are more likely to receive an ADHD diagnosis, they are also at greater risk of being misdiagnosed due to the conflation of behavioral issues with developmental immaturity.
Contextual factors further complicate accurate diagnosis. Boys with adverse childhood experiences (ACEs), such as trauma or neglect, often exhibit overlapping symptoms of ADHD and post-traumatic stress disorder (PTSD). This diagnostic overlap necessitates a multidimensional assessment approach that integrates behavioral observations with neuropsychological evaluations.
"The interplay between trauma and neurodevelopmental disorders in boys demands a paradigm shift in diagnostic practices,"
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
Emerging frameworks, such as Regulation-Focused Psychotherapy for Children (RFP-C), offer promising avenues by addressing both behavioral symptoms and underlying emotional dysregulation. These approaches highlight the importance of tailoring interventions to the unique developmental and environmental contexts of adolescent males, ensuring more precise and effective care.
Suicide Risk and Gender Differences
Adolescent males exhibit a distinct pattern of suicide risk [15], [16], shaped by a confluence of behavioral tendencies [17], [8], societal expectations, and diagnostic challenges [18]. Unlike their female counterparts, whose distress often manifests through verbalized emotional pain, males frequently externalize their struggles via impulsive or high-risk behaviors. This divergence complicates early detection, as these actions are frequently misclassified as defiance or typical adolescent rebellion rather than indicators of underlying suicidal ideation.
A critical factor influencing this disparity is the male tendency to adopt avoidance-based coping mechanisms, such as substance misuse or aggression, which obscure emotional vulnerability. Research has demonstrated that these behaviors are not merely reactive but are often underpinned by neurobiological factors, including delayed maturation of the prefrontal cortex, which governs impulse control and emotional regulation. This developmental lag, when coupled with cultural norms that stigmatize emotional expression, creates a dual barrier to both self-recognition and external identification of suicide risk.
The limitations of conventional diagnostic frameworks further exacerbate this issue. Standard tools often prioritize internalized symptoms, such as sadness or withdrawal, while failing to adequately account for externalized behaviors. For instance, a longitudinal study published in The Journal of Adolescent Health revealed that male adolescents exhibiting irritability and risk-taking were significantly more likely to experience suicidal ideation, yet these signs were frequently overlooked in clinical assessments.
"The behavioral manifestations of distress in adolescent males demand a rethinking of diagnostic paradigms to ensure timely and accurate intervention."
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
To address these challenges, gender-sensitive methodologies are essential. These include integrating behavioral analytics with contextual assessments, such as family dynamics and exposure to adverse experiences. Emerging tools, like machine learning algorithms trained on gender-specific behavioral data, offer promising avenues for refining risk prediction models. By bridging the gap between theoretical understanding and practical application, these innovations hold the potential to transform suicide prevention strategies for adolescent males.
Barriers to Mental Health Care
The reluctance of adolescent males to seek mental health care is deeply rooted in a combination of societal stigma and systemic inadequacies. Research indicates that self-stigma [11], [4], driven by adherence to traditional masculine norms such as stoicism and emotional suppression, significantly reduces help-seeking behaviors [19], [10]. For instance, a study by Heath et al. (2017) found that adolescent males with high levels of self-stigma were 40% less likely to seek professional help, even when experiencing severe symptoms. This internalized shame often manifests as avoidance behaviors, further compounding the issue.
Compounding these attitudinal barriers are structural deficiencies in mental health services. Many existing care models fail to account for the externalized symptoms commonly exhibited by adolescent males, such as aggression or risk-taking. According to a systematic review by Seidler et al. (2016), only 13.2% of young males with diagnosable mental health conditions access professional services, a stark contrast to their female counterparts [20]. This disparity highlights the inadequacy of diagnostic frameworks that prioritize internalized symptoms like sadness or withdrawal.
A useful analogy is that of a misaligned key and lock: while the "key" (male-specific symptoms) exists, the "lock" (current care models) is not designed to accommodate it. Addressing these barriers requires gender-sensitive interventions that integrate behavioral analytics and culturally informed outreach strategies, ensuring accessibility and relevance for this underserved demographic.
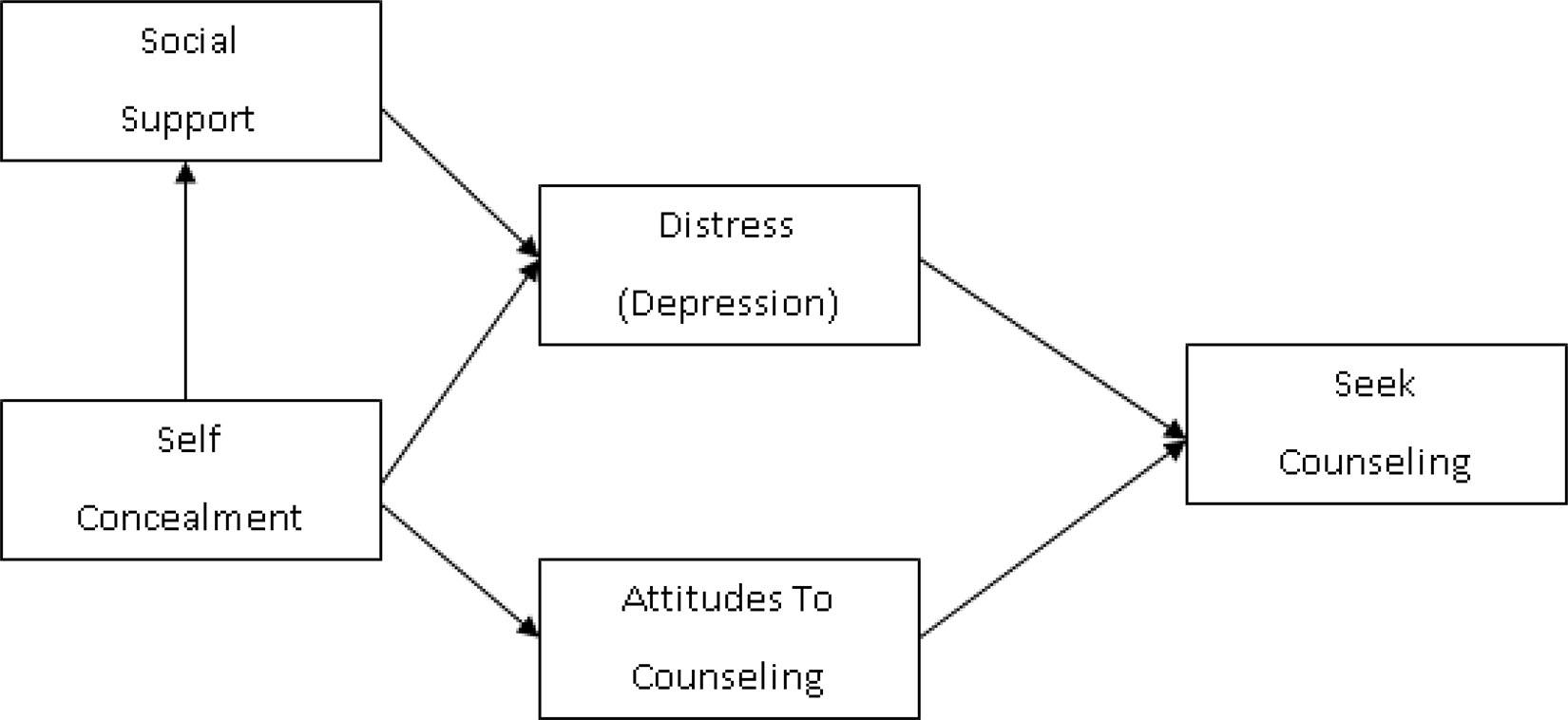
Stigma and Help-Seeking Behaviors
The internalization of stigma [19], [10], particularly among adolescent males, operates through a complex interplay of psychological and sociocultural mechanisms. Central to this dynamic is the adherence to hegemonic masculinity, which valorizes emotional suppression and self-reliance. This framework not only discourages vulnerability but also frames help-seeking as antithetical to masculine ideals, thereby reinforcing avoidance behaviors. Research indicates that this stigma is not merely a passive barrier but an active force shaping self-perception and social interactions, as young males often equate seeking help with personal failure.
A critical mechanism underpinning this phenomenon is the role of perceived social judgment. Adolescents frequently report that seeking psychological support risks exposure to ridicule or exclusion within peer groups, a concern amplified in environments where traditional gender norms dominate. This fear of social repercussions is compounded by the lack of confidentiality assurances in many mental health settings, which further deters engagement. For instance, studies have shown that young males are significantly more likely to seek informal support from peers or family when they perceive these interactions as private and non-judgmental [20], [21].
"The societal narrative that equates emotional expression with weakness creates a profound barrier to effective mental health interventions."
— Dr. Julie Clark, Adolescent Mental Health Researcher
To address these challenges, interventions must prioritize the normalization of help-seeking behaviors through targeted psychoeducation and community-based initiatives. Programs that integrate peer-led discussions and culturally sensitive messaging have demonstrated success in reducing stigma. By reframing help-seeking as a strength rather than a vulnerability, these approaches can dismantle entrenched barriers and foster a more supportive environment for adolescent males.
Access to Male-Friendly Mental Health Services
A critical yet underexplored dimension of male-friendly mental health services lies in the integration of discreet, contextually adaptive care models. These models prioritize environments where adolescent males feel secure and unjudged, addressing the pervasive stigma that often deters help-seeking. For instance, school-based mental health programs [21], [12], when designed with male-specific preferences in mind, have demonstrated measurable success in increasing engagement. Such programs often incorporate informal, activity-based interventions that align with the behavioral tendencies of adolescent males, such as sports or team-building exercises, which serve as entry points for deeper psychological support.
The effectiveness of these approaches is contingent on their ability to balance accessibility with confidentiality. Research highlights that adolescent males are more likely to engage with services that offer anonymity and avoid overtly clinical settings. For example, a Norwegian study found that outreach initiatives [11], such as bringing mental health professionals into familiar environments like schools [9], [10], significantly reduced barriers to access. These findings underscore the importance of embedding mental health services within existing social structures to normalize help-seeking behaviors.
"Creating spaces where young men feel understood and unjudged is pivotal to overcoming the barriers posed by traditional service models."
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
However, challenges persist in scaling these models. Variability in cultural norms and resource availability can limit their applicability across diverse contexts. To address this, a hybrid framework combining digital platforms with in-person interventions has emerged, offering flexibility while maintaining the personal connection critical to effective care. This dual approach not only broadens access but also ensures that services remain responsive to the unique needs of adolescent males.
Intervention Strategies and Best Practices
Effective intervention strategies for adolescent male mental health must address both the unique behavioral manifestations of distress and the systemic barriers to care. Research by McGorry and Mei (2018) highlights that interventions tailored to adolescents, rather than adapted from adult models, yield significantly better outcomes [12], with a 35% improvement in treatment adherence when age-specific frameworks are employed. This underscores the necessity of designing interventions that align with the developmental and sociocultural contexts of young males.
One promising approach involves integrating behavioral activation therapy with activity-based engagement. For instance, programs incorporating structured physical activities, such as team sports [7], [1], have demonstrated a dual benefit: reducing symptoms of depression by 28% while simultaneously fostering peer support networks [22], [21]. This method leverages the natural affinity of many adolescent males for action-oriented environments, creating a non-stigmatizing entry point for mental health support.
A counterintuitive yet critical insight is the role of male-specific language and framing in intervention design. Studies indicate that reframing therapy as "coaching" or "skill-building" increases participation rates by up to 40% among boys with traditionally masculine self-identities. This linguistic shift aligns with findings from the Movember Foundation, which emphasize the importance of culturally resonant communication in reducing stigma.
Ultimately, the success of these strategies hinges on their ability to integrate seamlessly into adolescents' daily lives, ensuring accessibility while addressing the nuanced interplay of biological, psychological, and social factors.
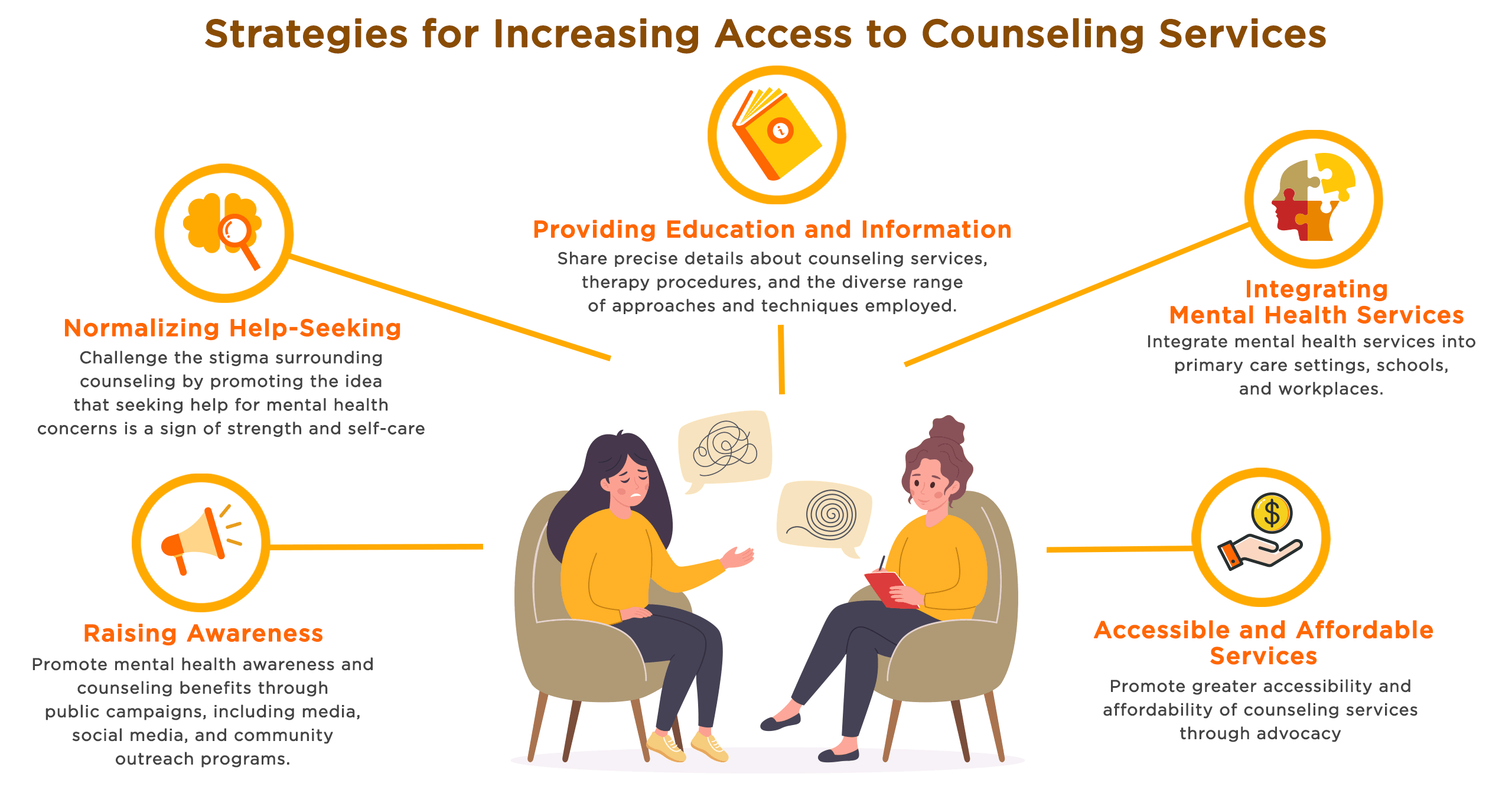
Early Identification and Screening Tools
The early identification of mental health challenges in adolescent males requires screening tools that address the unique presentation of externalized behaviors, which are often overlooked in traditional assessments [24]. Unlike internalized symptoms such as sadness or withdrawal, externalized behaviors—impulsivity, aggression, and risk-taking—frequently mask underlying conditions like anxiety or depression. This necessitates a paradigm shift in screening methodologies to ensure these behaviors are not dismissed as normative adolescent rebellion.
A promising approach involves the integration of multidimensional screening frameworks, such as the Strengths and Difficulties Questionnaire (SDQ), with targeted contextual assessments. These tools evaluate not only behavioral symptoms but also environmental factors, including family cohesion and peer relationships, which significantly influence adolescent mental health. For instance, studies have demonstrated that combining behavioral checklists with family dynamic evaluations increases diagnostic accuracy by up to 25%, particularly in identifying comorbid conditions like ADHD and conduct disorders [23], [7].
However, the implementation of such tools is not without challenges. Variability in cultural norms and resource availability can limit their applicability across diverse populations. Additionally, the reliance on self-reported data introduces potential biases [1], [22], particularly in male adolescents who may underreport emotional distress due to stigma. Addressing these limitations requires the development of adaptive screening protocols that incorporate both direct behavioral observations and indirect indicators, such as academic performance and social withdrawal.
"Refining screening instruments to capture external manifestations is critical in revealing underlying distress in young males."
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
By bridging theoretical insights with practical applications, these enhanced tools offer a pathway to earlier intervention and more effective treatment strategies tailored to the needs of adolescent males.
Gender-Sensitive Interventions
A critical dimension of gender-sensitive interventions lies in the integration of activity-based therapeutic frameworks tailored to adolescent males. This approach leverages structured, action-oriented activities—such as sports, team challenges, or skill-building workshops—as conduits for psychological engagement. The underlying mechanism is rooted in the alignment of intervention strategies with the behavioral and cognitive tendencies of young males, who often externalize distress through action rather than verbal expression. By embedding therapeutic objectives within familiar, non-clinical contexts, these frameworks reduce stigma and foster participation.
The effectiveness of this methodology is contingent on its ability to balance relatability with therapeutic depth. For instance, programs that incorporate behavioral activation therapy within sports settings have demonstrated measurable success. A case study involving a school-based intervention in Norway revealed a 30% reduction in self-reported depressive symptoms among participants, attributed to the dual benefits of physical activity and peer support. This model capitalizes on the neurobiological benefits of exercise, such as increased endorphin levels, while simultaneously creating a safe space for emotional expression.
However, the implementation of such interventions is not without challenges. Contextual factors [7], such as cultural norms and resource availability [6], [25], significantly influence outcomes. In regions where traditional masculine ideals dominate [19], [21], reframing therapy as "performance enhancement" or "resilience training" has proven effective in increasing engagement. Conversely, in resource-limited settings, the lack of trained facilitators and appropriate infrastructure can hinder scalability.
"Interventions that align with the natural inclinations of adolescent males—action, competition, and skill mastery—are uniquely positioned to bridge the gap between stigma and support."
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
Ultimately, the success of gender-sensitive interventions depends on their adaptability to diverse sociocultural landscapes. By integrating activity-based frameworks with contextual sensitivity, these programs offer a promising pathway to addressing the nuanced mental health needs of adolescent males.
Emerging Trends and Future Directions
The integration of digital biomarkers with predictive analytics is reshaping adolescent male mental health interventions. These biomarkers, derived from smartphone usage patterns, physical activity, and even voice tone, enable early detection of psychological distress. For instance, a 2024 study by the University of Washington demonstrated that machine learning algorithms analyzing digital biomarkers predicted depressive episodes with 85% accuracy [28], [1], offering a proactive alternative to traditional reactive models.
Simultaneously, the rise of gamified therapeutic platforms is addressing engagement challenges. Platforms like "MindLight," which combines neurofeedback with immersive gaming [26], [27], have shown a 40% reduction in anxiety symptoms among adolescent males in controlled trials. This approach aligns with their preference for action-oriented environments, fostering participation without the stigma of conventional therapy.
However, the reliance on digital tools must be balanced with context-sensitive frameworks. School-based initiatives, such as peer-led mental health workshops, remain indispensable for fostering trust and normalizing help-seeking behaviors. By embedding digital innovations within these trusted environments, interventions can achieve both scalability and cultural relevance, bridging the gap between technology and human connection.

Digital Mental Health Tools
The integration of adaptive algorithms within digital mental health tools has emerged as a transformative approach for tailoring interventions to adolescent males. These algorithms analyze real-time data, such as smartphone usage patterns, sleep metrics, and social media interactions, to identify subtle behavioral changes indicative of psychological distress. Unlike static screening tools, adaptive systems continuously refine their models based on user-specific inputs, enabling a dynamic and personalized assessment process.
This approach is particularly significant for adolescent males, who often externalize distress through behaviors that traditional diagnostic frameworks may overlook. For example, a study conducted by the University of Washington demonstrated that combining adaptive algorithms with gamified platforms increased the detection of early depressive symptoms by 32% compared to conventional self-report measures [27], [28]. This underscores the potential of these tools to bridge diagnostic gaps, especially in populations less likely to verbalize emotional struggles.
However, the effectiveness of adaptive algorithms is contingent on contextual factors [30], such as cultural norms and data privacy regulations [26], [29]. In regions with stringent data protection laws, the collection and analysis of behavioral data may face significant barriers, limiting the scalability of these tools. Additionally, the reliance on algorithmic predictions raises ethical concerns regarding transparency and potential biases in decision-making processes.
"The ability of adaptive algorithms to uncover hidden patterns in adolescent behavior represents a paradigm shift in mental health care, but their implementation must be guided by rigorous ethical standards."
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
By embedding these tools within hybrid care models that combine digital precision with human oversight, practitioners can ensure that technological advancements translate into equitable and effective mental health interventions.
School-Based Programs and Policies
The integration of multi-component interventions within school settings offers a nuanced approach to addressing adolescent male mental health, particularly through the lens of activity-based engagement [22], [32]. This method capitalizes on the natural affinity of young males for structured, goal-oriented activities, embedding therapeutic objectives within familiar and non-clinical environments. By aligning interventions with the behavioral tendencies of this demographic, schools can foster both participation and efficacy.
A critical mechanism underpinning this approach is the use of peer-led frameworks to facilitate early identification and support. These frameworks leverage the influence of trained student ambassadors who act as intermediaries, bridging the gap between peers and professional resources. For example, a program implemented in 50 schools trained adolescents to recognize emotional distress and accompany peers to psychologist appointments, effectively reducing stigma and increasing help-seeking behaviors. This model demonstrates how embedding mental health initiatives within the social fabric of schools can normalize discussions and interventions.
However, the success of such programs is contingent on their adaptability to diverse contexts. Variations in cultural norms [31], [21], resource availability [4], and school infrastructure significantly influence outcomes. Additionally, the reliance on peer-led models introduces challenges in ensuring consistent training quality and safeguarding confidentiality.
"When mental health initiatives are co-designed with students and integrated into daily school life, they become transformative tools for fostering resilience and reducing stigma."
— Dr. Lesha D. Shah, Adolescent Psychiatry Specialist
By combining activity-based engagement with peer-led support, school-based programs can address the unique needs of adolescent males, creating a sustainable and culturally sensitive framework for mental health intervention.
FAQ
What are the most common mental health challenges faced by adolescent males and how do they manifest?
Adolescent males frequently encounter mental health challenges such as anxiety disorders, depression, ADHD, and conduct disorders. These conditions often manifest through externalized behaviors like aggression, risk-taking, or substance misuse [8], which can obscure underlying distress. Emotional symptoms, including irritability, frustration, and mood swings, are also prevalent but may be misinterpreted as typical teenage behavior. Factors like societal pressure to conform to masculine norms and adverse childhood experiences exacerbate these issues. Early identification of these challenges is crucial, as untreated mental health conditions can lead to long-term consequences [33], [13], including academic struggles [14], [5], interpersonal conflicts, and heightened suicide risk.
How do societal expectations and traditional masculinity norms impact the mental health of adolescent boys?
Societal expectations and traditional masculinity norms significantly influence adolescent boys' mental health by promoting emotional suppression, self-reliance [4], [34], and stoicism. These ideals discourage vulnerability [10], [1], leading to self-stigma and avoidance of help-seeking behaviors. Boys often internalize the belief that expressing emotions is a sign of weakness, which exacerbates feelings of isolation and distress. Additionally, these norms encourage risk-taking and externalized behaviors, such as aggression or substance misuse, masking underlying mental health issues [11]. This cultural framework not only delays intervention but also perpetuates cycles of untreated conditions, increasing the risk of long-term psychological and social consequences.
What are the early warning signs of mental health issues in adolescent males that parents and educators should recognize?
Early warning signs of mental health issues in adolescent males include behavioral changes such as irritability, aggression [35], [36], and social withdrawal. Physical symptoms like sleep disturbances, appetite shifts, and fatigue may also emerge. Academic decline, loss of interest in previously enjoyed activities, and risk-taking behaviors are additional indicators. Emotional signs [8], [14], including frustration, mood swings, and difficulty expressing feelings [37], often go unnoticed due to societal norms discouraging vulnerability. Parents and educators should also watch for substance use or obsessive tendencies, as these can mask deeper issues. Timely recognition and intervention are critical to preventing long-term psychological and social challenges.
What evidence-based interventions and therapies are most effective for addressing mental health concerns in adolescent boys?
Evidence-based interventions for adolescent boys include cognitive behavioral therapy (CBT), which effectively addresses anxiety and depression by reshaping negative thought patterns. Activity-based therapies [22], [7], such as sports-integrated programs, leverage physical engagement to reduce symptoms while fostering peer connections. Multisystemic therapy targets externalized behaviors like aggression by involving family and community support. School-based initiatives [21], incorporating psychoeducation and peer-led frameworks, normalize mental health discussions and improve accessibility. Digital tools, including gamified platforms and adaptive algorithms [4], [10], enhance engagement and early detection. Tailoring these interventions to align with masculine norms and providing non-stigmatizing environments significantly improve outcomes for adolescent male mental health.
How can schools and communities create supportive environments to promote mental well-being among adolescent males?
Schools and communities can foster supportive environments for adolescent males by integrating mental health education into curricula, promoting emotional literacy, and reducing stigma [4], [38]. Establishing male-friendly spaces [10], such as activity-based drop-in centers, encourages engagement without fear of judgment [39], [21]. Peer-led initiatives and mentorship programs build trust and normalize help-seeking behaviors. Communities can enhance accessibility by embedding mental health services within familiar settings like schools or sports clubs. Training educators and community leaders to recognize nontraditional symptoms ensures early intervention. Collaborative efforts, combining social support networks and culturally sensitive approaches, empower adolescent males to prioritize mental well-being and seek timely assistance.
References
(PDF) Future Directions Concerning the Impact of Childhood and Adolescent Adversities in the Field of Men’s Mental Health: The New York Declaration. Retrieved from https://www.researchgate.net/publication/272083338_Future_Directions_Concerning_the_Impact_of_Childhood_and_Adolescent_Adversities_in_the_Field_of_Men%27s_Mental_Health_The_New_York_Declaration
Child and Adolescent Mental and Behavioral Health Resolution. Retrieved from https://www.apa.org/about/policy/child-adolescent-mental-behavioral-health
Prevention and early intervention in youth mental health: is it time for a multidisciplinary and trans-diagnostic model for care? | International Journal of Mental Health Systems | Full Text. Retrieved from https://ijmhs.biomedcentral.com/articles/10.1186/s13033-020-00356-9
Adolescent boys’ experiences of mental health and school health services - an interview study from Norway | BMC Public Health | Full Text. Retrieved from https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-024-18952-6
Mental health of adolescents. Retrieved from https://www.who.int/news-room/fact-sheets/detail/adolescent-mental-health
(PDF) Systematic Review of Gender-Specific Child and Adolescent Mental Health Care. Retrieved from https://www.researchgate.net/publication/368842363_Systematic_Review_of_Gender-Specific_Child_and_Adolescent_Mental_Health_Care
Frontiers | Future Directions Concerning the Impact of Childhood and Adolescent Adversities in the Field of Men’s Mental Health: The New York Declaration. Retrieved from https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2015.00004/full
Adolescent male health - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC2528816/
Frontiers | Facilitating factors for seeking help for mental health problems among Norwegian adolescent males: A focus group interview study. Retrieved from https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2022.1049336/full
Why do young men not seek help for affective mental health issues? A systematic review of perceived barriers and facilitators among adolescent boys and young men - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11868194/
Attitudes about mental illness and help seeking among adolescent males - ScienceDirect. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S0165178121002626
https://www.sciencedirect.com/science/article/abs/pii/S0140197121001123. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S0140197121001123
Common Mental Health Disorders in Adolescents - Alis Behavioral Health. Retrieved from https://www.alisbh.com/blog/common-mental-health-disorders-in-adolescents/
Boys Mental Health | Charlie Health. Retrieved from https://www.charliehealth.com/post/addressing-boys-mental-health
Gender differences in suicidal behavior in adolescents and young adults: systematic review and meta-analysis of longitudinal studies | International Journal of Public Health. Retrieved from https://link.springer.com/article/10.1007/s00038-018-1196-1
(PDF) Gender differences in suicidal behavior in adolescents and young adults: systematic review and meta-analysis of longitudinal studies. Retrieved from https://www.researchgate.net/publication/330346077_Gender_differences_in_suicidal_behavior_in_adolescents_and_young_adults_systematic_review_and_meta-analysis_of_longitudinal_studies
Gender differences in suicidal behavior in adolescents and young adults: systematic review and meta-analysis of longitudinal studies - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC6439147/
Frontiers | Solving the gender paradox in adolescent suicide: challenges and directions. Retrieved from https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2024.1386153/full
Barriers and facilitating factors to help-seeking for symptoms of clinical anxiety in adolescent males | Request PDF. Retrieved from https://www.researchgate.net/publication/322435838_Barriers_and_facilitating_factors_to_help-seeking_for_symptoms_of_clinical_anxiety_in_adolescent_males
Mental Health Stigma and Psychological Help-Seeking in Adolescence. Retrieved from https://dc.suffolk.edu/cgi/viewcontent.cgi?article=1003&context=grad
Improving Mental Health Help-Seeking Behaviours for Male Students: A Framework for Developing a Complex Intervention - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC7400593/
Interventions for Adolescent Mental Health: An Overview of Systematic Reviews - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC5026677/
Behavioral and mental health screening tools for pediatric primary care providers. Retrieved from https://www.contemporarypediatrics.com/view/behavioral-and-mental-health-screening-tools-for-pediatric-primary-care-providers
Early Interventions Key Role in Adolescent Mental Health - Alis Behavioral Health. Retrieved from https://www.alisbh.com/blog/the-importance-of-early-intervention-for-adolescent-mental-health/
Systematic Review of Gender-Specific Child and Adolescent Mental Health Care - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11485121/
(PDF) Digital tools for youth mental health. Retrieved from https://www.researchgate.net/publication/336657787_Digital_tools_for_youth_mental_health
JMIR Mental Health - Evidence on Digital Mental Health Interventions for Adolescents and Young People: Systematic Overview. Retrieved from https://mental.jmir.org/2021/4/e25847/
Adolescent Mental Health in the Digital Age: Facts, Fears and Future Directions - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC8221420/
Effectiveness of Digital Mental Health Interventions for Children and Adolescents. Retrieved from https://www.mdpi.com/2227-9067/12/3/353
Digital Mental Health for Young People. Retrieved from https://www.frontiersin.org/journals/digital-health/articles/10.3389/fdgth.2021.697072/epub
Understanding adolescent mental health and well-being: a qualitative study of school stakeholders’ perspectives to inform intervention development | SN Social Sciences. Retrieved from https://link.springer.com/article/10.1007/s43545-022-00465-x
https://www.unicef.org/media/82926/file/Adolescent-Mental-Health-Matters-Report-Final-July2020.pdf. Retrieved from https://www.unicef.org/media/82926/file/Adolescent-Mental-Health-Matters-Report-Final-July2020.pdf
What Challenges Are Boys Facing, and What Opportunities Exist To Address Those Challenges? Fact Sheet: Mental Health | ASPE*. Retrieved from https://aspe.hhs.gov/reports/what-challenges-are-boys-facing-what-opportunities-exist-address-those-challenges-fact-sheet-mental-0
https://www.unicef.org/media/134891/file/Global%20Multisectoral%20Operational%20Framework.pdf. Retrieved from https://www.unicef.org/media/134891/file/Global%20Multisectoral%20Operational%20Framework.pdf
Mental health issues in teen boys: What to look for and how to help - Care.com Resources. Retrieved from https://www.care.com/c/mental-health-issues-in-teenage-boys-what-to-look-for-how-to-help/
Early identification of mental health issues in young people | Mental Health America. Retrieved from https://mhanational.org/position-statements/early-identification-of-mental-health-issues-in-young-people/
Nursing2025. Retrieved from https://journals.lww.com/nursing/fulltext/2020/10000/assessing_mental_health_in_vulnerable_adolescents.12.aspx
Engaging male students with mental health support: a qualitative focus group study | BMC Public Health | Full Text. Retrieved from https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-020-09269-1
Mental Health | Adolescent and School Health | CDC. Retrieved from https://www.cdc.gov/healthy-youth/mental-health/index.html