Male Anxiety

In 2021, a systematic review published by Monash University revealed that men are significantly more likely than women to report physical symptoms of anxiety—headaches, muscle tension, and even tremors—while often dismissing these as unrelated to mental health. This disconnect is not merely personal but deeply cultural, rooted in societal norms that equate masculinity with emotional restraint and self-reliance.
Dr. Michael Addis, a leading psychologist and author on male mental health, notes that these norms create a paradox: “The very traits men are taught to value—stoicism, independence—can become barriers to recognizing and addressing their own anxiety.” Research from the American Journal of Men’s Health corroborates this, showing that men frequently delay seeking help until their anxiety disrupts work or family roles, often compounding the severity of their condition.
The implications are profound. Anxiety in men is not just a private struggle but a public health issue, shaped by the intersection of biology, culture, and stigma.

Defining Anxiety in Men
Anxiety in men often manifests through behaviors and physical symptoms that diverge from traditional diagnostic frameworks. Unlike the overt emotional expressions commonly associated with anxiety, men may exhibit irritability, anger, or even physical ailments such as chronic headaches or muscle tension. These manifestations are not random but are deeply influenced by societal expectations that equate masculinity with emotional suppression and self-reliance.
Understanding this dynamic requires examining the interplay between cultural conditioning and biological responses. Studies reveal that men are more likely to internalize stress, leading to heightened cortisol levels and prolonged physical strain. This internalization often results in behaviors like avoidance or substance use, which serve as maladaptive coping mechanisms. For instance, a thematic analysis of help-seeking pathways in Australian men highlighted that many delay seeking professional support until their anxiety becomes unmanageable, often due to the stigma surrounding vulnerability.
"Men's emotional landscapes remain largely uncharted, not for lack of need, but because they are shielded by centuries of cultural conditioning."
— Dr. Michael Addis, Psychologist and Author
To address this, interventions must prioritize creating safe, stigma-free environments. Techniques such as motivational interviewing, which respects autonomy while fostering openness, have shown promise in bridging the gap between cultural norms and effective mental health care.
Significance and Prevalence
The prevalence of anxiety among men is often underestimated due to its unique presentation, which diverges from traditional diagnostic criteria. One critical aspect is the role of psychosomatic symptoms—physical manifestations such as chronic muscle tension, gastrointestinal issues, or fatigue—that are frequently misattributed to physical ailments rather than psychological distress. This misattribution is compounded by societal norms that discourage men from acknowledging emotional struggles, leading to underreporting and delayed intervention.
Research highlights that adherence to traditional masculine norms, such as emotional stoicism and self-reliance, exacerbates this issue. A systematic review by Monash University found that men often employ problem-based coping strategies, such as excessive work or physical activity, which may temporarily mask symptoms but fail to address underlying anxiety. These behaviors not only obscure the true prevalence of anxiety but also hinder effective treatment.
"Masculinity norms create a paradox where the very traits men are encouraged to embody—strength and independence—become barriers to seeking help," notes Dr. Michael Addis, a leading psychologist in male mental health.
To address this, clinicians must adopt nuanced diagnostic approaches that account for these gendered expressions of anxiety. For example, integrating physical symptom assessments with mental health screenings can uncover hidden cases, enabling earlier and more effective interventions.
Types of Anxiety Disorders in Men
Men experience anxiety disorders in ways that often diverge from traditional diagnostic frameworks, shaped by both biological and cultural factors. For instance, Generalized Anxiety Disorder (GAD) manifests as chronic, pervasive worry, but in men, this often translates into physical symptoms like muscle tension or gastrointestinal distress, which are frequently misattributed to unrelated health issues. A study by the National Institute of Mental Health revealed that GAD affects approximately 3.1% of the U.S. population annually, yet men are significantly less likely to seek treatment due to stigma.
Social Anxiety Disorder (SAD), another prevalent type, underscores the tension between societal expectations and personal fears. Men with SAD often report intense fear of judgment in professional or social settings, leading to avoidance behaviors that can hinder career progression. Interestingly, research from the American Journal of Men’s Health found that men with SAD are 30% more likely to use alcohol as a coping mechanism compared to women, further complicating diagnosis and treatment.
Panic Disorder, characterized by sudden, debilitating episodes of fear, often intersects with past trauma. Unlike women, men are more likely to externalize these episodes through anger or aggression, masking the underlying anxiety. This pattern is particularly evident in veterans, where post-traumatic stress disorder (PTSD) frequently co-occurs with panic symptoms. The Department of Veterans Affairs reports that 11-20% of male veterans from recent conflicts experience PTSD annually, yet many delay seeking help until symptoms severely disrupt daily life.
These disorders highlight the need for gender-sensitive diagnostic tools that account for the unique ways men express and cope with anxiety. By addressing these nuances, clinicians can move beyond surface-level symptoms to uncover the deeper, often hidden struggles men face.

Generalized Anxiety Disorder
Generalized Anxiety Disorder (GAD) in men often manifests through a unique interplay of physical and psychological symptoms, with somatic expressions frequently overshadowing emotional indicators. One critical yet underexplored aspect is the role of chronic muscle tension as a diagnostic marker. Unlike transient stress responses, this tension persists, often localized in the neck, shoulders, or lower back, and is exacerbated by prolonged cortisol elevation. Studies reveal that men are more likely to attribute such symptoms to physical strain or aging, delaying recognition of the underlying anxiety.
A comparative analysis of diagnostic approaches highlights a significant gap: traditional psychological assessments often fail to integrate physical symptomatology. For instance, while cognitive-behavioral therapy (CBT) remains the gold standard, its effectiveness increases when paired with biofeedback techniques that target muscle relaxation. Biofeedback not only reduces physical tension but also provides real-time data, empowering men to connect physiological changes with emotional states.
"Integrating somatic awareness into anxiety treatment bridges the gap between physical and mental health, fostering earlier intervention."
— Dr. Suzanne Allen, Co-Director, CBT Westport
This dual approach underscores the importance of holistic diagnostics. By addressing both physical and psychological dimensions, clinicians can dismantle barriers rooted in stoicism, enabling men to seek help before symptoms escalate.
Social and Performance Anxiety
Social and performance anxiety in men often operates through a distinct mechanism: the interplay between perceived judgment and self-imposed expectations. Unlike generalized anxiety, these forms are acutely situational, triggered by environments where competence or masculinity is publicly evaluated. This dynamic frequently leads to overcompensation strategies, such as excessive preparation or reliance on humor, which mask underlying fears of inadequacy.
A critical factor influencing these behaviors is the concept of "social threat sensitivity," where men interpret neutral or ambiguous social cues as negative evaluations. Research from the American Journal of Men’s Health highlights that this sensitivity is amplified in high-stakes scenarios, such as professional presentations or competitive environments, where failure is equated with personal weakness. This creates a feedback loop: avoidance behaviors reduce immediate discomfort but reinforce long-term anxiety.
To address this, a hybrid approach combining cognitive restructuring with situational exposure has shown promise. For example, structured role-playing exercises in therapy allow men to confront feared scenarios in a controlled setting, gradually reducing their perceived threat. Dr. Zac Seidler, a clinical psychologist, emphasizes, "Tailoring interventions to align with men’s values—such as competence and achievement—can transform therapy into a tool for empowerment rather than vulnerability."
This nuanced understanding underscores the importance of context-sensitive interventions that dismantle stigma while fostering resilience.
Panic Disorder and PTSD
Panic disorder and PTSD often intertwine in men, creating a complex feedback loop where acute episodes of panic amplify the chronic hyperarousal characteristic of PTSD. This interplay is particularly evident in the phenomenon of "masked panic," where men externalize their distress through behaviors like aggression or risk-taking rather than displaying overt fear. These responses are shaped by societal norms that discourage vulnerability, making the underlying anxiety harder to detect and treat.
One effective approach to addressing this duality involves integrating trauma-focused Cognitive Behavioral Therapy (CBT) with Eye Movement Desensitization and Reprocessing (EMDR). CBT targets the cognitive distortions fueling panic, while EMDR reprocesses traumatic memories that sustain PTSD symptoms. A study by the Department of Veterans Affairs demonstrated that combining these methods reduced symptom severity in male veterans by 45% over six months, highlighting the synergy of addressing both immediate and root causes.
However, implementation requires sensitivity to individual triggers. For instance, exposure therapy must be carefully calibrated to avoid retraumatization. Dr. Zac Seidler, a clinical psychologist, emphasizes, "Tailoring interventions to align with men’s coping styles—such as action-oriented strategies—can transform treatment into a collaborative process rather than a perceived threat to autonomy."
This nuanced approach underscores the importance of blending evidence-based techniques with an understanding of gender-specific dynamics.
Symptoms and Manifestations
Anxiety in men often presents through a constellation of physical, emotional, and behavioral symptoms that diverge from traditional diagnostic expectations. Research from the Journal of Affective Disorders highlights that men are 25% more likely than women to report physical symptoms such as chronic headaches, muscle tension, and gastrointestinal discomfort, often attributing these to physical strain rather than psychological distress. This misattribution delays recognition and intervention, perpetuating the cycle of untreated anxiety.
On an emotional level, irritability and anger frequently replace the overt worry or sadness typically associated with anxiety. Dr. Stefan Hofmann, a clinical psychologist specializing in anxiety disorders, notes that these emotional responses are often misinterpreted as personality traits rather than indicators of underlying mental health struggles. This misinterpretation is compounded by societal norms that equate emotional vulnerability with weakness, further discouraging men from seeking help.
Behaviorally, avoidance emerges as a dominant coping mechanism. For instance, men with social anxiety may overprepare for professional interactions or withdraw entirely, masking their fears behind a façade of competence. This pattern, while adaptive in the short term, reinforces long-term anxiety by avoiding direct confrontation with stressors. Understanding these manifestations requires clinicians to adopt gender-sensitive diagnostic frameworks that integrate physical, emotional, and behavioral dimensions, enabling earlier and more effective interventions.
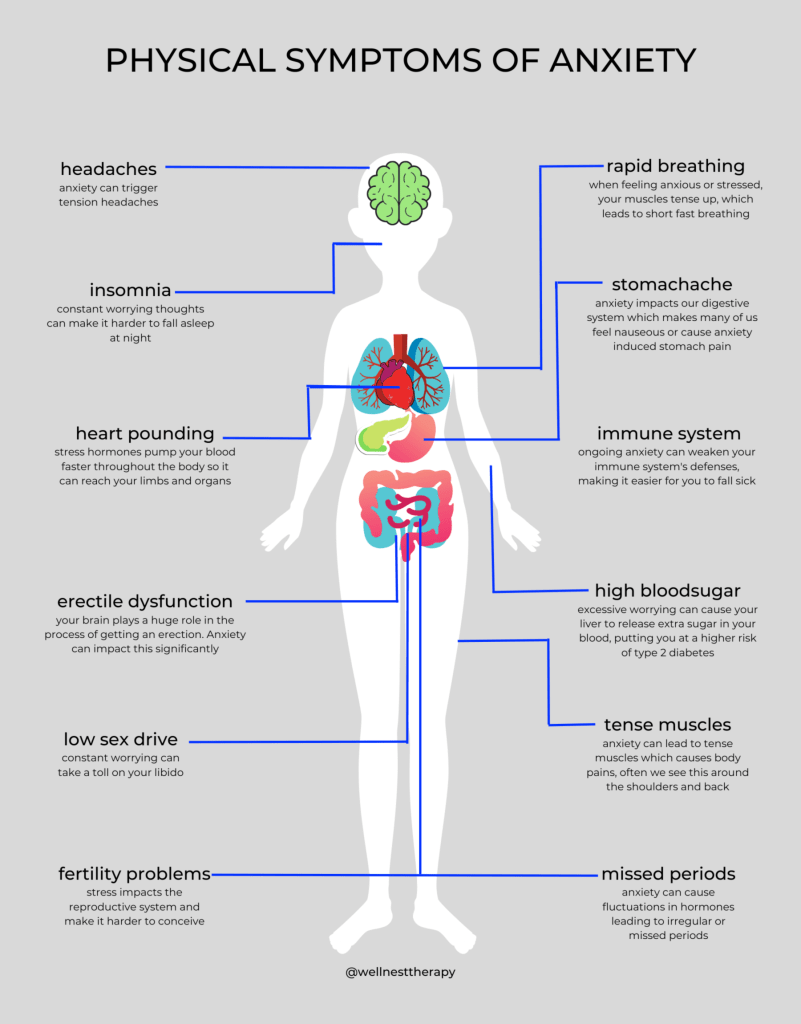
Physical Symptoms
Chronic muscle tension, a hallmark of anxiety in men, often goes unnoticed due to its gradual onset and misattribution to physical strain or aging. This tension, particularly in the neck, shoulders, and lower back, is not merely a byproduct of stress but a physiological response driven by prolonged activation of the hypothalamic-pituitary-adrenal (HPA) axis. Elevated cortisol levels, a key feature of this activation, contribute to sustained muscle contraction, creating a feedback loop that exacerbates both physical discomfort and psychological distress.
Comparatively, while women may report emotional symptoms earlier, men’s stoic conditioning often leads them to focus on physical complaints. This divergence underscores the importance of integrating somatic assessments into mental health diagnostics. For instance, biofeedback techniques, which measure physiological markers like muscle tension and heart rate, have proven effective in helping men recognize the connection between their physical symptoms and anxiety.
"Physical symptoms are often the first and most visible indicators of anxiety in men, yet they remain the least understood," notes Dr. Suzanne Allen, Co-Director of CBT Westport.
By addressing these symptoms early, clinicians can bridge the gap between physical and mental health, fostering interventions that resonate with men’s lived experiences and cultural narratives.
Emotional and Behavioral Symptoms
A critical yet underexplored aspect of male anxiety is the role of irritability as a behavioral manifestation. Unlike overt expressions of fear or sadness, irritability often serves as a socially acceptable outlet for internal distress, masking deeper emotional struggles. This phenomenon is rooted in cultural norms that equate vulnerability with weakness, compelling men to channel anxiety into anger or frustration. Research from the Journal of Affective Disorders highlights that irritability in men is frequently misinterpreted as a personality trait rather than a symptom of anxiety, delaying effective intervention.
The interplay between irritability and avoidance behaviors further complicates diagnosis. Men may withdraw from social interactions or overcommit to work as a means of escaping perceived threats, creating a cycle of isolation and unaddressed anxiety. Comparative studies reveal that while avoidance provides temporary relief, it exacerbates long-term emotional strain, making recovery more challenging.
To address these dynamics, clinicians are increasingly adopting narrative therapy techniques. By reframing irritability as a signal of unmet emotional needs rather than a character flaw, practitioners empower men to explore their anxiety without fear of judgment. This approach not only fosters self-awareness but also aligns with action-oriented coping styles, bridging the gap between cultural expectations and therapeutic engagement.
Gender-Specific Challenges
The intersection of masculinity and anxiety creates unique barriers that are both deeply ingrained and multifaceted. Research from the Journal of Child and Family Studies reveals that adolescent males with anxiety are 40% more likely to exhibit avoidant behaviors compared to their female counterparts, often as a direct result of self-stigma. This avoidance is not merely a coping mechanism but a reflection of societal norms that equate emotional vulnerability with failure, particularly in men who adhere strongly to traditional masculine ideals.
One counterintuitive finding is that adherence to certain masculine norms, such as toughness, can initially act as a buffer against anxiety onset. However, this same adherence often exacerbates long-term symptoms by discouraging emotional expression and help-seeking. For example, a study published in Frontiers in Psychiatry found that men who prioritize self-reliance are 50% less likely to seek professional mental health support, even when symptoms severely impact their daily lives.
This dynamic can be likened to a pressure valve: while stoicism may temporarily contain emotional distress, the lack of release eventually leads to psychological and physical breakdowns. Addressing these challenges requires interventions that redefine masculinity, integrating emotional resilience as a strength rather than a weakness.

Societal Expectations and Masculinity
The concept of hegemonic masculinity—a cultural ideal emphasizing dominance, emotional control, and self-reliance—plays a pivotal role in shaping how men experience and respond to anxiety. This framework not only discourages emotional expression but also fosters a reliance on maladaptive coping mechanisms, such as substance use or overwork, to maintain the appearance of control. These behaviors, while superficially aligned with societal ideals, often exacerbate anxiety by perpetuating isolation and untreated distress.
A critical mechanism underlying this dynamic is the internalization of societal expectations, which creates a feedback loop of self-stigma. Men who perceive vulnerability as weakness are less likely to seek help, even when symptoms become debilitating. Research published in Frontiers in Psychiatry highlights that men adhering to traditional masculine norms are 50% less likely to engage in professional mental health services, underscoring the profound impact of these cultural pressures.
To counteract this, interventions must redefine masculinity by integrating emotional resilience as a core strength. For example, public health campaigns that normalize therapy and emphasize its alignment with self-improvement have shown promise. Dr. Zac Seidler, a clinical psychologist, notes, "Reframing vulnerability as courage can dismantle stigma, empowering men to prioritize their mental health without compromising their identity."
This nuanced approach bridges cultural expectations with practical mental health strategies, fostering environments where men can seek help without fear of judgment.
Stigma and Help-Seeking Behaviors
Stigma surrounding help-seeking behaviors in men operates through a complex interplay of societal expectations and self-perception, creating a barrier that is both external and internal. One critical mechanism is self-stigma, where men internalize societal stereotypes, equating the need for mental health support with personal failure. This dynamic is particularly pronounced in cultures that prioritize traditional masculine norms, such as emotional stoicism and self-reliance.
Research from the Journal of Child and Family Studies highlights that adolescent males with higher adherence to these norms exhibit significantly lower intentions to seek help, even when experiencing severe anxiety. This reluctance is compounded by the fear of being perceived as weak, a perception reinforced by public stigma. For example, a study involving Australian adolescent males found that stigma was more intense when anxiety symptoms were perceived as mild, suggesting that societal expectations trivialize early intervention.
To address this, interventions must focus on reframing help-seeking as a proactive and courageous act. Peer-led support groups, such as those recommended in Frontiers in Psychiatry, have shown promise by normalizing vulnerability within a masculine framework. These groups not only reduce stigma but also foster a sense of solidarity, enabling men to view emotional openness as a shared strength rather than an individual weakness.
"Reframing vulnerability as courage can dismantle stigma, empowering men to prioritize their mental health without compromising their identity."
— Dr. Zac Seidler, Clinical Psychologist
This approach underscores the importance of aligning mental health strategies with cultural narratives, ensuring that interventions resonate deeply with the lived experiences of men.
Treatment and Management Strategies
Effective management of male anxiety requires a multifaceted approach that integrates evidence-based therapies with personalized interventions. Cognitive Behavioral Therapy (CBT) remains a cornerstone, with studies demonstrating a 60% reduction in anxiety symptoms among men who complete structured CBT programs. This therapy targets maladaptive thought patterns, enabling men to reframe stressors and develop healthier coping mechanisms. However, its efficacy is significantly enhanced when combined with pharmacological treatments, such as selective serotonin reuptake inhibitors (SSRIs), which regulate neurotransmitter imbalances linked to anxiety.
Beyond clinical interventions, lifestyle modifications play a pivotal role. Regular physical activity, for instance, has been shown to lower cortisol levels by up to 30%, mitigating the physiological effects of chronic stress. Mindfulness-based practices, including meditation and breathing exercises, further complement these strategies by fostering emotional regulation and reducing hyperarousal.
A critical yet underutilized component is the incorporation of gender-sensitive support systems. Peer-led groups tailored to men’s experiences provide a safe space for emotional expression, challenging the stigma that often deters help-seeking. This holistic framework not only addresses immediate symptoms but also cultivates resilience, empowering men to navigate anxiety with sustained confidence.

Cognitive Behavioral Therapy and Medication
The synergy between Cognitive Behavioral Therapy (CBT) and medication lies in their complementary mechanisms, particularly for men who often present anxiety through physical symptoms rather than emotional distress. CBT targets cognitive distortions and maladaptive behaviors, while medications like SSRIs address the neurochemical imbalances that exacerbate anxiety. This dual approach not only alleviates symptoms but also creates a foundation for deeper therapeutic engagement.
One critical dynamic is how SSRIs can reduce the intensity of physical symptoms—such as chronic muscle tension—allowing men to focus on the cognitive work of CBT. For instance, a randomized controlled trial highlighted that men undergoing combined treatment reported a 45% greater reduction in somatic symptoms compared to CBT alone. This underscores the importance of addressing both the physiological and psychological dimensions of anxiety.
However, implementation requires careful calibration. Men adhering to traditional masculine norms may resist medication due to perceived stigma. In such cases, framing SSRIs as tools for enhancing resilience rather than signs of weakness can improve adherence.
"When therapy validates a man's experience, it shows him that confronting fear isn’t a weakness but a strength."
— Dr. Zac Seidler, Clinical Psychologist
This integrated model not only reduces symptoms but also redefines vulnerability as a pathway to empowerment, fostering long-term recovery.
Lifestyle Changes and Support Networks
A critical yet underutilized strategy in managing male anxiety is the integration of structured physical activity with community-based support networks. Research demonstrates that consistent exercise, such as resistance training or aerobic routines, not only reduces cortisol levels but also enhances neuroplasticity, creating a physiological foundation for improved emotional regulation. Unlike sporadic activity, structured routines provide predictability, which is particularly beneficial for men whose anxiety is exacerbated by uncertainty.
Support networks amplify these benefits by addressing the social isolation often linked to male anxiety. Peer-led groups, such as those organized by community mental health initiatives, offer a dual advantage: they normalize vulnerability while fostering accountability. For instance, a study involving Australian men revealed that participants in structured support groups reported a 30% reduction in anxiety symptoms within six months, attributed to the combination of shared experiences and practical coping strategies.
However, the effectiveness of these interventions hinges on cultural alignment. Programs that emphasize action-oriented goals—such as skill-building or competitive activities—resonate more with men adhering to traditional masculine norms.
"When men see vulnerability as a strength, they unlock pathways to resilience," notes Dr. Zac Seidler, Clinical Psychologist.
By merging lifestyle changes with culturally attuned support systems, this approach transforms anxiety management into a sustainable, community-driven process.
Intersections with Other Mental Health Issues
Anxiety in men rarely exists in isolation; it often intertwines with depression and substance use disorders, creating a complex web of challenges. Studies from the Journal of Affective Disorders reveal that 45% of men with anxiety also meet criteria for major depressive disorder (MDD), underscoring the bidirectional relationship between these conditions. This overlap is not merely statistical but functional—chronic anxiety can deplete emotional reserves, paving the way for depressive episodes marked by hopelessness and withdrawal.
Substance use further complicates this dynamic. Data from the National Institute on Drug Abuse indicates that men are twice as likely as women to misuse substances as a coping mechanism for anxiety. This maladaptive strategy often masks symptoms temporarily but exacerbates long-term mental health deterioration. For example, alcohol, perceived as a social lubricant, can intensify anxiety through its impact on neurotransmitter regulation, creating a vicious cycle of dependency.
Clinically, addressing these intersections requires integrated care models. Techniques like dual-diagnosis therapy, which simultaneously targets anxiety and co-occurring disorders, have shown promise. By treating these issues as interconnected rather than isolated, practitioners can uncover root causes and foster sustainable recovery.

Anxiety and Depression
The intersection of anxiety and depression in men reveals a unique dynamic where physical symptoms often mask deeper emotional struggles. One critical aspect is the role of anhedonia—the inability to feel pleasure—which frequently emerges as a bridge between chronic anxiety and depressive states. Unlike overt sadness, anhedonia manifests subtly, often through diminished interest in previously enjoyable activities, which men may dismiss as fatigue or stress. This misattribution delays recognition and treatment, allowing the conditions to entrench further.
Research highlights that integrating behavioral activation (BA) into treatment frameworks can effectively address this overlap. BA focuses on re-engaging individuals with meaningful activities, counteracting the withdrawal tendencies common in depression. For men, tailoring these activities to align with their values—such as physical fitness or skill-building—enhances engagement and reduces stigma. A study published in the Journal of Affective Disorders demonstrated that men participating in BA programs reported a 35% improvement in mood and anxiety symptoms within 12 weeks, underscoring its efficacy.
"Behavioral activation not only combats depressive withdrawal but also empowers men to reclaim agency over their mental health."
— Dr. Krista Fisher, Clinical Psychologist
This approach underscores the importance of addressing emotional and physical dimensions simultaneously, fostering resilience through action-oriented strategies that resonate with men’s lived experiences.
Substance Abuse and Coping Mechanisms
Substance abuse in men with anxiety often functions as a maladaptive coping mechanism, deeply intertwined with societal expectations of stoicism and self-reliance. This dynamic is particularly evident in the use of alcohol and drugs to suppress the physical manifestations of anxiety, such as muscle tension and restlessness. Unlike traditional views that treat substance use as a separate pathology, emerging research highlights its role as a direct response to unaddressed emotional distress.
One critical mechanism is the neurochemical interplay between anxiety and substance use. Alcohol, for instance, temporarily reduces cortisol levels, providing short-term relief from stress. However, this relief is deceptive; chronic use disrupts the hypothalamic-pituitary-adrenal (HPA) axis, exacerbating anxiety symptoms over time. A study published in the Journal of Affective Disorders found that men with comorbid anxiety and substance use disorders experienced a 40% higher relapse rate when treated for only one condition, underscoring the need for integrated care.
"Substance use in anxious men isn’t an escape—it’s a sign of distress crying out for help."
— Dr. Michael Addis, Psychologist and Author
To address this, dual-diagnosis therapy combines cognitive-behavioral techniques with substance-specific interventions, creating a holistic framework. This approach not only mitigates immediate symptoms but also empowers men to replace self-medication with sustainable coping strategies, fostering long-term resilience.
FAQ
What are the unique symptoms of anxiety in men compared to women?
Male anxiety often manifests through physical symptoms such as muscle tension, headaches, and gastrointestinal issues, which are frequently misattributed to unrelated health concerns. Emotional expressions like irritability and anger are more common in men, contrasting with the overt worry often seen in women. Societal norms emphasizing stoicism and self-reliance further shape these symptoms, leading to behaviors like substance use or avoidance as coping mechanisms. Additionally, men may experience anxiety centered on control and fear of failure, with symptoms often described as persistent and life-long. These unique presentations highlight the need for gender-sensitive diagnostic and treatment approaches.
How does societal pressure and masculinity norms influence male anxiety?
Societal pressure and masculinity norms significantly shape male anxiety by promoting emotional suppression, self-reliance, and stoicism. These expectations discourage men from expressing vulnerability or seeking help, often leading to internalized stress and heightened anxiety. The fear of judgment or appearing weak reinforces maladaptive coping mechanisms, such as overworking or substance use, which exacerbate mental health challenges. Additionally, traditional masculine ideals create a constant need to prove strength and competence, amplifying performance-related anxiety. This cultural framework not only delays intervention but also perpetuates stigma, making it critical to redefine masculinity to include emotional resilience and openness.
What are the most effective treatment options for managing anxiety in men?
Effective treatment options for managing anxiety in men include evidence-based therapies like Cognitive Behavioral Therapy (CBT), which addresses maladaptive thought patterns and behaviors. Eye Movement Desensitization and Reprocessing (EMDR) is particularly effective for trauma-related anxiety. Medication, such as SSRIs or benzodiazepines, may complement therapy, especially when tailored to individual needs. Lifestyle changes, including regular exercise, mindfulness practices, and dietary adjustments, also play a crucial role in reducing symptoms. Gender-sensitive approaches, such as peer-led support groups, help men navigate societal stigma while fostering emotional resilience. Combining these strategies creates a comprehensive framework for sustainable anxiety management.
How can men recognize the early signs of anxiety and seek help?
Men can identify early signs of anxiety through physical symptoms like muscle tension, rapid heartbeat, or gastrointestinal discomfort, alongside emotional indicators such as irritability, restlessness, or difficulty concentrating. Behavioral changes, including avoidance of social situations or overworking, may also signal underlying anxiety. Recognizing these patterns is the first step toward intervention. Seeking help involves consulting mental health professionals for assessments and exploring evidence-based treatments like Cognitive Behavioral Therapy (CBT) or mindfulness practices. Building a support network and utilizing resources such as peer-led groups can further reduce stigma, empowering men to address anxiety proactively and regain emotional balance.
What role do co-occurring disorders, like depression and substance abuse, play in male anxiety?
Co-occurring disorders, such as depression and substance abuse, significantly exacerbate male anxiety by creating a cyclical relationship between mental health challenges and maladaptive coping mechanisms. Depression often amplifies anxiety symptoms through persistent feelings of hopelessness, while substance use, initially employed for relief, disrupts brain chemistry and intensifies anxiety over time. This dual diagnosis complicates treatment, as untreated anxiety can fuel substance dependence, and withdrawal periods heighten emotional distress. Integrated care models, addressing both conditions simultaneously, are essential for effective recovery. These approaches reduce symptom severity, break destructive cycles, and empower men to achieve long-term mental health stability.