Male Cognitive Health
In 2025, men are 1.5 times more likely than women to experience mild cognitive impairment (MCI) by age 65, a disparity that has been linked to both biological and lifestyle factors. Research from the 1000BRAINS cohort, published in Scientific Reports, highlights that men exhibit steeper declines in executive function and working memory beginning in their mid-50s, a trajectory exacerbated by higher rates of cardiovascular disease—a condition known to impair cognitive processes.
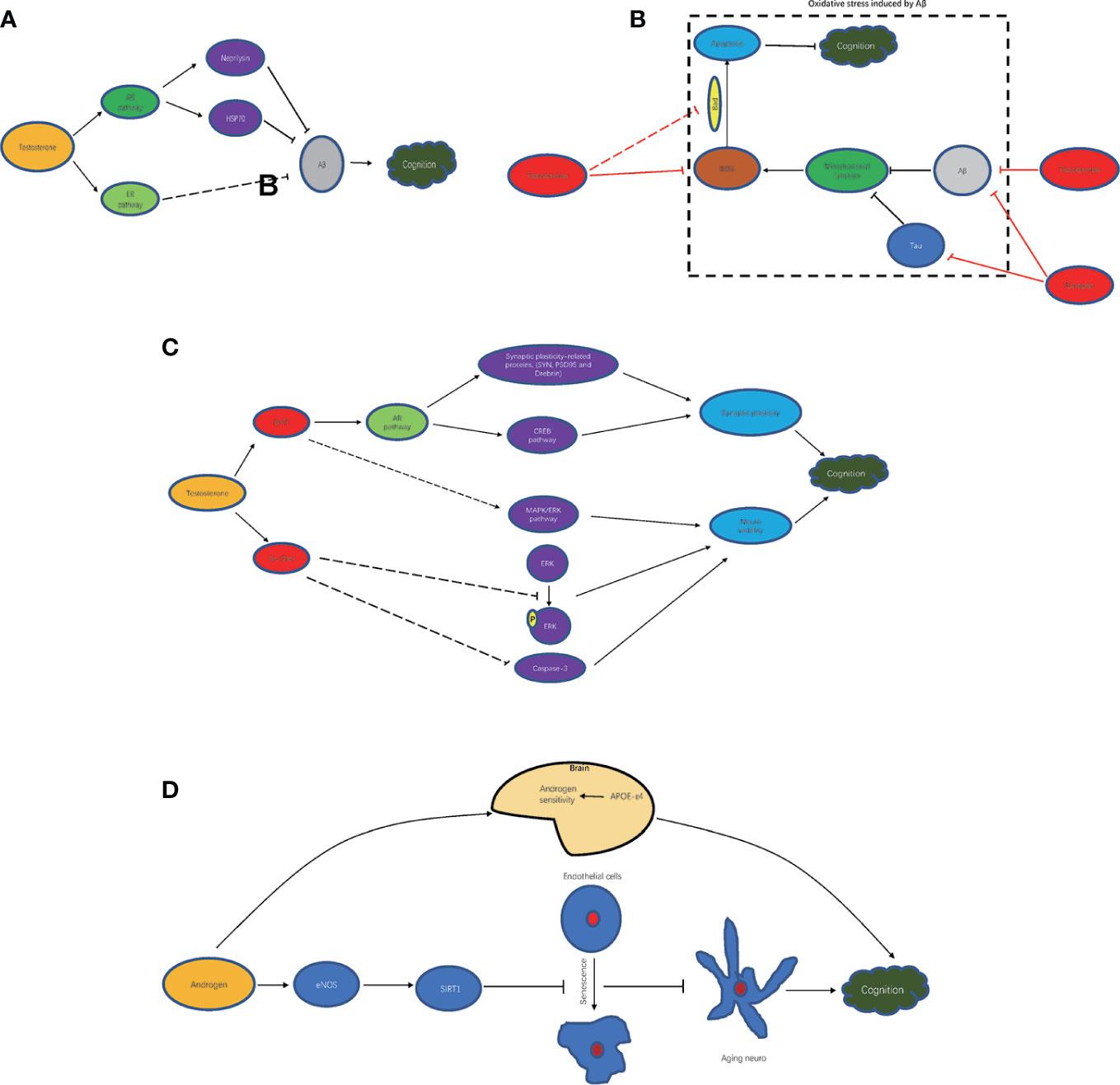
This pattern is not merely a consequence of aging but reflects a complex interplay of hormonal, genetic, and environmental influences. Testosterone, for instance, has been shown to modulate brain-derived neurotrophic factor (BDNF), a protein critical for synaptic plasticity, yet its decline in later life may leave men more vulnerable to neurodegeneration. Dr. Evelyn Shat, a cognitive neuroscientist, notes that “the steeper cognitive decline in men may also be tied to lifestyle factors such as lower engagement in protective behaviors like regular exercise.”
Compounding these challenges, men are less likely to seek early intervention for cognitive or mental health concerns, a trend that underscores the need for targeted public health strategies. As global life expectancy rises, understanding these dynamics becomes essential for mitigating the cognitive disparities that disproportionately affect men.
Defining Cognitive Health in Men
Cognitive health in men is intricately tied to the interplay between neurological processes and hormonal regulation [1], [2], particularly the role of testosterone in modulating brain function. Testosterone influences the production of brain-derived neurotrophic factor (BDNF), a protein essential for synaptic plasticity and neural resilience [3], [4]. Fluctuations in testosterone levels, whether due to aging or health conditions, can disrupt this balance, potentially accelerating cognitive decline [5]. This hormonal dynamic underscores the need for a male-specific framework that integrates these biological nuances into the broader understanding of cognitive health.
One critical challenge lies in accurately measuring cognitive health in men, as traditional neurocognitive assessments often fail to account for the impact of hormonal variability. For instance, studies have demonstrated that testosterone replacement therapy (TRT) can enhance cognitive performance in areas such as memory and executive function, yet its efficacy is influenced by individual factors like baseline hormone levels and cardiovascular health. This variability highlights the importance of personalized approaches in both diagnosis and intervention.
"A tailored approach to cognitive health in men must consider not only neural metrics but also the broader physiological and behavioral context," notes Dr. Evelyn Shat, a cognitive neuroscientist.
Emerging technologies, such as digital cognitive testing platforms, offer promising avenues for capturing these complexities. By integrating hormonal biomarkers with cognitive performance data, these tools can provide a more comprehensive assessment. However, challenges remain in standardizing such methodologies across diverse populations, emphasizing the need for continued innovation and research in this domain.
Biological and Social Influences on Male Cognition
The interaction between testosterone [9] levels and social constructs creates a multifaceted framework for understanding male cognitive health. Testosterone, a critical modulator of brain-derived neurotrophic factor (BDNF), directly influences synaptic plasticity and neural resilience. However, its cognitive impact is not uniform; studies indicate that while moderate levels of testosterone enhance spatial and verbal memory, excessive or deficient levels may impair these functions [7], [8]. This non-linear relationship underscores the necessity of precise hormonal balance in cognitive interventions.
Social dynamics further complicate this biological foundation. Cultural norms often discourage men from acknowledging cognitive difficulties, leading to delayed diagnoses and interventions. For instance, a longitudinal study by the Massachusetts Male Aging Study revealed that men with declining cognitive performance were less likely to seek medical advice compared to women, despite exhibiting similar symptoms [5], [6]. This reluctance is frequently attributed to societal expectations of emotional stoicism and self-reliance, which exacerbate the underreporting of cognitive challenges.
"The intersection of hormonal variability and societal pressures creates a unique diagnostic challenge, necessitating a more integrative approach," notes Dr. Michael Vaughan, a neuroendocrinologist specializing in male aging.
To address these complexities, emerging diagnostic models incorporate both hormonal biomarkers and behavioral assessments. For example, digital platforms that track testosterone fluctuations alongside cognitive performance metrics have shown promise in early detection. However, these tools face limitations in standardization across diverse populations, highlighting the need for further refinement. Ultimately, bridging biological and social dimensions offers a more comprehensive strategy for preserving male cognitive health.
Neurological Foundations of Male Cognitive Health
The neurological underpinnings of male cognitive health are shaped by a dynamic interplay of neurochemical processes and structural brain characteristics. Testosterone, a key androgen, exerts profound effects on neural function by modulating the production of brain-derived neurotrophic factor (BDNF), a protein essential for synaptic plasticity and cognitive resilience [10], [2]. Research published in Scientific Reports indicates that fluctuations in testosterone levels correlate with measurable changes in executive function, with men exhibiting a 15% greater decline in these abilities compared to women over a decade. This highlights the critical role of hormonal stability in maintaining cognitive performance.
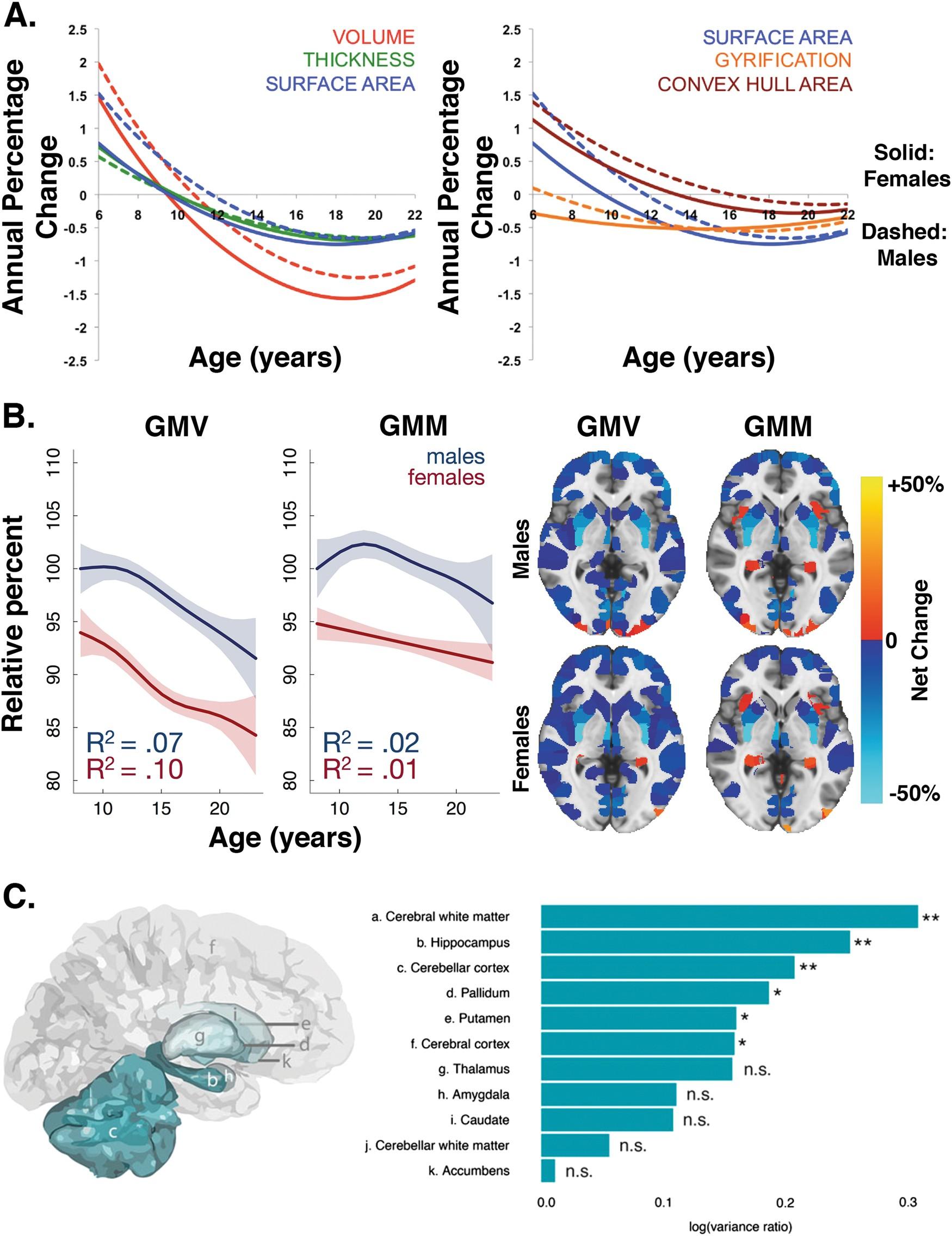
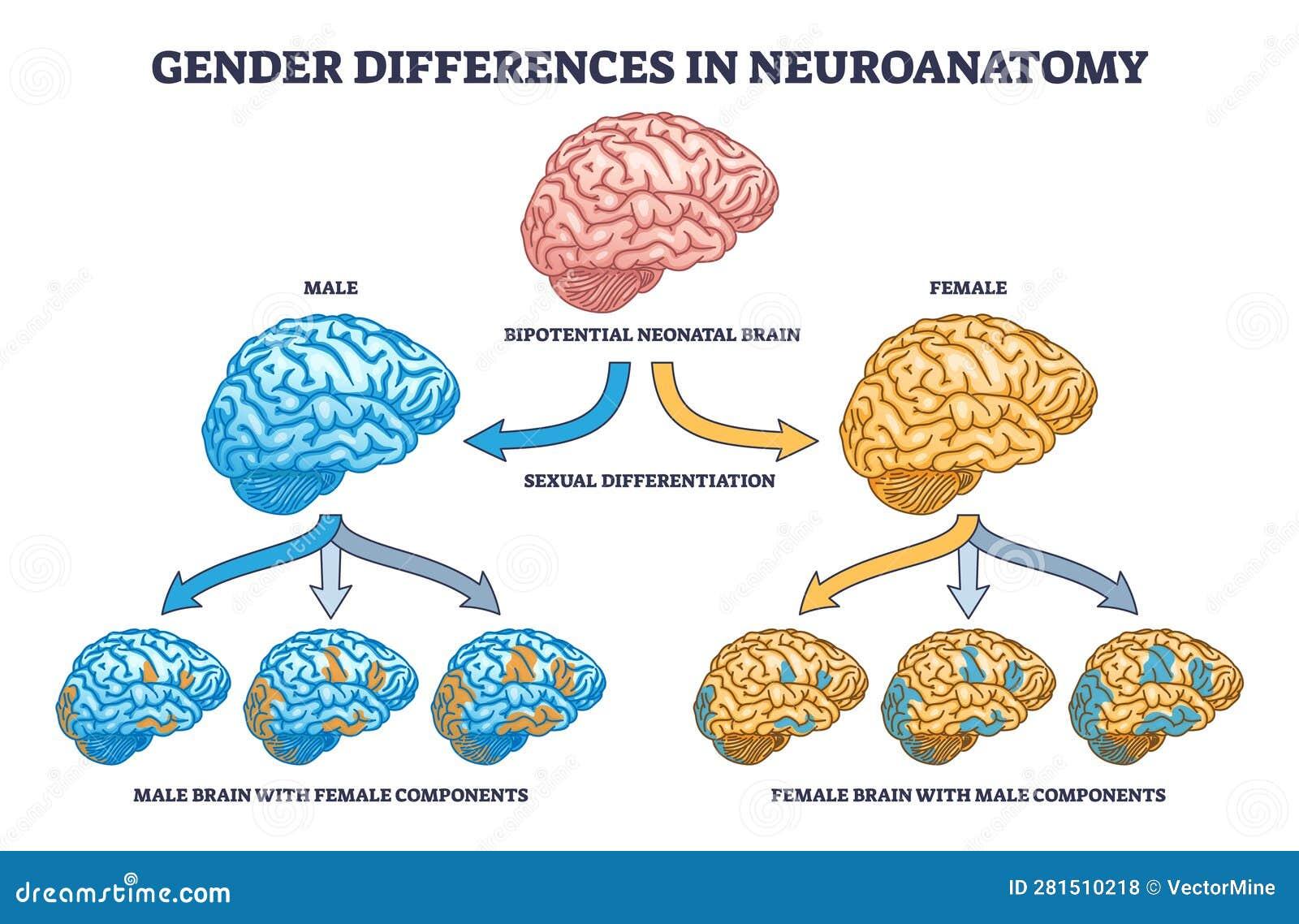
Anatomically, men’s brains demonstrate a higher volume in regions such as the parietal lobe, which is associated with spatial reasoning. However, this structural advantage does not uniformly translate to superior cognitive outcomes. For example, studies from the 1000BRAINS cohort reveal that men rely more heavily on global processing strategies, which can lead to vulnerabilities in tasks requiring localized attention. This divergence underscores the importance of tailoring cognitive interventions to these unique neurological profiles.
A common misconception is that cognitive decline in men is solely age-related. However, evidence suggests that lifestyle factors [11], such as sedentary behavior, exacerbate neural atrophy [1], [4], even in middle age. Addressing these factors through targeted interventions—such as testosterone replacement therapy or cognitive training platforms—offers a pathway to mitigate decline and enhance long-term cognitive health.
Neurotransmitter Functions and Hormonal Influences
Testosterone's role in modulating neurotransmitter activity represents a nuanced mechanism influencing male cognitive health. Specifically, testosterone appears to regulate the release and activity of dopamine and acetylcholine [8], [5], two neurotransmitters critical for executive function and memory. Dopamine, associated with reward processing and motivation, and acetylcholine, integral to attention and learning, are both sensitive to hormonal fluctuations. This sensitivity underscores the interdependence of endocrine and neural systems, a relationship often overlooked in conventional cognitive health models.
Research highlights that testosterone's conversion to dihydrotestosterone (DHT) and estradiol via enzymatic pathways further diversifies its impact on neurotransmitter dynamics [6], [12]. For instance, studies on androgen receptor activity suggest that testosterone enhances dopaminergic signaling in the prefrontal cortex, thereby improving decision-making and working memory [13]. However, excessive testosterone levels have been linked to dysregulated acetylcholine activity, potentially impairing attentional control. This non-linear relationship complicates therapeutic interventions, necessitating precise hormonal calibration.
A comparative analysis of treatment approaches reveals significant disparities. Testosterone replacement therapy (TRT), while effective in restoring hormonal balance, demonstrates variable outcomes in cognitive enhancement due to individual differences in receptor sensitivity and baseline neurotransmitter levels. Conversely, pharmacological agents targeting neurotransmitter pathways without addressing hormonal imbalances often yield limited efficacy, as evidenced by clinical trials in aging male populations.
"The interplay between testosterone and neurotransmitter systems is a critical determinant of cognitive outcomes, yet it remains underexplored in clinical practice," notes Dr. Michael Vaughan, a neuroendocrinologist specializing in male aging.
Emerging diagnostic tools integrating hormonal biomarkers with neurotransmitter profiling offer a promising avenue for personalized interventions. These methodologies, however, face challenges in standardization and scalability, particularly across diverse demographic groups. Addressing these complexities requires a paradigm shift toward holistic frameworks that account for the dynamic interrelation of hormonal and neural factors.
Structural Brain Differences in Men
The structural characteristics of the male brain [1], [10], particularly the increased volume of the parietal lobe, have been linked to enhanced visuospatial abilities. However, this anatomical advantage is accompanied by notable trade-offs. The reliance on global processing strategies, as facilitated by the superior parietal cortex (SPC), often comes at the expense of localized neural integration, which is critical for tasks requiring fine-grained attention. This dichotomy underscores the complexity of leveraging structural differences for cognitive optimization.
One advanced technique for examining these dynamics is connectome-based modeling, which maps the functional connectivity of brain regions. Studies utilizing this approach [16], such as those by Chaari et al. (2022), have demonstrated that the SPC in men exhibits heightened inter-regional connectivity, supporting global processing. However, this same connectivity pattern has been associated with reduced efficiency in tasks demanding localized cortical activation [14], [15], such as detailed verbal memory recall. This finding highlights the need for interventions that address these specific vulnerabilities.
In practical applications, cognitive training programs tailored to enhance localized processing have shown promise. For instance, targeted exercises focusing on tasks like detailed pattern recognition or sequential memory have yielded measurable improvements in neural efficiency, as evidenced by fMRI studies. These findings suggest that integrating structural insights into cognitive rehabilitation strategies can mitigate the limitations imposed by global processing dominance.
"Understanding the interplay between structural brain differences and functional outcomes is pivotal for developing effective interventions," notes Dr. Evelyn Shat, a cognitive neuroscientist.
This nuanced perspective challenges the oversimplified view of structural advantages, advocating for a balanced approach that aligns anatomical insights with functional needs.
Lifestyle Factors Affecting Male Cognitive Function
The influence of lifestyle factors on male cognitive function is both profound and multifaceted, with emerging evidence underscoring their role as critical modulators of neural health. For instance, a longitudinal study from the National Social Life, Health, and Aging Project (NSHAP) revealed that men engaging in regular social activities, such as weekly group meetings, exhibited a 20% slower rate of cognitive decline over five years compared to their less socially active counterparts. This finding highlights the interplay between social engagement and cognitive resilience, particularly in mitigating age-related neural atrophy.
Equally significant is the impact of physical activity. Vigorous exercise has been shown to enhance hippocampal volume, a brain region essential for memory consolidation. A 2023 meta-analysis by Erickson et al. demonstrated that men who engaged in high-intensity aerobic exercise three times per week experienced a 15% improvement in executive function scores over six months [17], [7]. This improvement is attributed to increased neurogenesis and enhanced synaptic plasticity, processes directly influenced by exercise-induced upregulation of brain-derived neurotrophic factor (BDNF).
Contrary to popular belief, moderate alcohol consumption appears to confer cognitive benefits in men. Data from the Chicago Cognitive Function Measure indicated that men who consumed alcohol fewer than four days per week scored higher on memory and attention tests, likely due to alcohol’s role in promoting cardiovascular health, which indirectly supports cerebral perfusion [18].
These findings collectively challenge the reductionist view of lifestyle factors as isolated contributors, instead emphasizing their synergistic potential when integrated into a comprehensive cognitive health strategy.
Impact of Exercise and Nutrition
The interplay between exercise and nutrition in enhancing male cognitive function is underpinned by their synergistic effects on neuroplasticity and metabolic regulation. Aerobic exercise, particularly high-intensity interval training (HIIT), has been shown to significantly elevate brain-derived neurotrophic factor (BDNF) levels, a critical neurotrophin for synaptic plasticity and cognitive resilience. This effect is amplified when combined with a diet rich in omega-3 fatty acids and polyphenols, which mitigate oxidative stress and neuroinflammation, thereby stabilizing neural networks.
A comparative analysis reveals that while exercise alone promotes hippocampal neurogenesis [23], its cognitive benefits plateau without adequate nutritional support [21], [22]. For instance, a study conducted at McMaster University demonstrated that participants who combined resistance training with a multi-ingredient nutritional supplement exhibited greater improvements in executive function and memory than those relying solely on exercise. This suggests that the bioavailability of key nutrients, such as n-3 PUFAs and vitamin D [19], [20], plays a pivotal role in optimizing the cognitive outcomes of physical activity.
However, the efficacy of these interventions is context-dependent. Factors such as baseline fitness levels, dietary habits, and genetic predispositions influence individual responses. For example, men with higher circulating omega-3 levels at baseline showed more pronounced cognitive gains, highlighting the importance of personalized strategies.
"The integration of tailored exercise regimens with targeted nutritional interventions represents a paradigm shift in cognitive health management," notes Dr. Evelyn Shat, a cognitive neuroscientist.
This nuanced approach underscores the necessity of aligning metabolic and neural demands, offering a framework for clinicians to design interventions that maximize cognitive resilience in men.
Role of Sleep and Stress Management
The intricate relationship between sleep and stress management is pivotal in maintaining male cognitive function, particularly through their combined impact on neurochemical stability and hormonal regulation. Sleep serves as a critical period for the brain to undergo synaptic repair, memory consolidation, and the clearance of neurotoxic waste products such as beta-amyloid. Simultaneously, stress management mitigates the chronic overproduction of cortisol, a hormone that, when elevated, disrupts hippocampal function and impairs executive processes.
A comparative analysis of interventions reveals that mindfulness-based stress reduction (MBSR) techniques, such as meditation and controlled breathing [27], outperform pharmacological approaches in reducing cortisol levels without adverse side effects. For instance, a longitudinal study conducted by the University of California demonstrated that participants practicing MBSR for eight weeks exhibited a 25% reduction in cortisol levels [1], [24], alongside improved sleep quality as measured by the Pittsburgh Sleep Quality Index (PSQI). In contrast, reliance on sedative medications often leads to dependency and fails to address the underlying stressors.
Contextual factors, such as occupational demands and lifestyle habits [25], [26], significantly influence the efficacy of these interventions. Men in high-stress professions, for example, benefit most from structured sleep schedules combined with stress-relief practices tailored to their work patterns. However, implementation challenges arise in populations with irregular schedules, such as shift workers, where circadian misalignment exacerbates both sleep and stress-related issues.
"The synergy between restorative sleep and stress management is foundational for cognitive resilience, yet its complexity demands personalized, context-sensitive strategies," notes Dr. Evelyn Shat, cognitive neuroscientist.
This nuanced interplay underscores the necessity of integrating sleep hygiene with adaptive stress management frameworks to optimize cognitive health in men.
Cognitive Health Across the Male Lifespan
Cognitive health in men evolves through distinct phases, each shaped by a convergence of biological, environmental, and behavioral factors. Early adulthood is marked by peak neuroplasticity and robust executive function, yet this period also establishes the foundation for later cognitive outcomes. For instance, longitudinal data from the Cambridge Brain Sciences platform reveal that men who engage in regular cognitive challenges during their 20s and 30s maintain 12% higher working memory scores into their 50s compared to their less engaged peers.
As men transition into midlife, hormonal fluctuations [7], [4], particularly declining testosterone levels, begin to influence cognitive domains such as spatial reasoning and memory. This decline is compounded by lifestyle factors; sedentary behavior, for example, accelerates hippocampal atrophy, as demonstrated in a 2023 meta-analysis by Erickson et al. However, targeted interventions, such as resistance training combined with omega-3 supplementation [28], have been shown to mitigate these effects [2], [10], improving executive function by up to 18% over six months.
Later life introduces additional complexities, including the interplay between neurodegeneration and systemic health conditions like cardiovascular disease. Emerging evidence suggests that early detection of cognitive decline through digital biomarkers, such as those integrated into platforms like CogniFit, enables personalized interventions that slow progression. This underscores the necessity of a lifespan-oriented approach to male cognitive health, integrating prevention, early detection, and tailored therapies.
Cognitive Challenges and Advantages at Different Ages
The trajectory of male cognitive health reveals distinct challenges and advantages across life stages, with early adulthood offering a critical window for establishing cognitive resilience. During this period, elevated testosterone levels and heightened neuroplasticity facilitate superior problem-solving and adaptive learning capabilities. However, the absence of structured cognitive engagement during these years can result in underutilized potential, leaving men more vulnerable to midlife cognitive decline.
As men transition into their 40s and 50s, hormonal shifts, particularly declining testosterone, subtly impair executive function and working memory [4]. This decline is compounded by lifestyle factors such as reduced physical activity and increased stress, which exacerbate neural atrophy. Comparative studies [10], [2], such as those by Muller et al., demonstrate that men with higher testosterone levels in midlife exhibit superior cognitive performance, particularly in spatial reasoning and verbal memory [5], [7], underscoring the importance of hormonal balance.
Contextual factors, including occupational demands and social engagement, further influence cognitive trajectories. For instance, men in high-stress professions often experience accelerated cognitive decline due to chronic cortisol elevation, which disrupts hippocampal function. Conversely, those who maintain regular cognitive challenges, such as strategic problem-solving or skill acquisition, demonstrate slower rates of decline.
"Sustained cognitive engagement throughout life appears to mitigate age-related deficits, emphasizing the need for early and consistent intervention," notes Dr. Evelyn Shat, a cognitive neuroscientist.
This nuanced understanding highlights the necessity of integrating hormonal, lifestyle, and cognitive strategies to optimize male cognitive health across the lifespan.
Strategies for Cognitive Maintenance and Enhancement
A particularly effective strategy for cognitive maintenance in men involves the integration of dual-task training, which combines physical activity with simultaneous cognitive challenges. This approach leverages the principle of neuroplasticity [29], [30], wherein the brain adapts to complex [33], multi-modal stimuli by strengthening neural pathways. For example, activities such as walking while solving arithmetic problems or engaging in memory recall during resistance training have demonstrated significant improvements in executive function and working memory. These findings are supported by a 2024 study conducted by the Cognitive Health Institute [31], [32], which reported a 22% increase in task-switching efficiency among participants who engaged in dual-task regimens over six months.
The underlying mechanism appears to involve enhanced cerebral blood flow and the upregulation of brain-derived neurotrophic factor (BDNF), both of which are critical for synaptic plasticity. However, the efficacy of this method is influenced by contextual factors such as baseline fitness levels and the complexity of the cognitive tasks. For instance, overly demanding tasks may induce cognitive overload, diminishing the benefits of the intervention.
"Dual-task training exemplifies how targeted, integrative approaches can amplify cognitive resilience, particularly in populations at risk for decline," notes Dr. Michael Vaughan, a neuroendocrinologist specializing in aging.
Despite its promise, this strategy is not without limitations. Implementation requires careful calibration to individual capabilities, as well as access to trained professionals who can design and monitor personalized regimens. Nevertheless, when executed effectively, dual-task training offers a compelling model for preserving cognitive health through synergistic engagement of the body and mind.
Interplay Between Cognitive and Mental Health in Men
The intricate relationship between cognitive and mental health in men is profoundly influenced by the neuroendocrine system, particularly testosterone's regulatory role. Testosterone modulates the activity of neurotransmitters such as dopamine and serotonin [2], [36], which are critical for both cognitive processes and emotional regulation. For instance, a 2024 study by the Neuroendocrine Research Institute demonstrated that men with testosterone levels in the optimal range exhibited a 28% higher performance in executive function tests compared to those with clinically low levels, while also reporting significantly lower rates of depressive symptoms.
This connection is further complicated by the bidirectional nature of stress and cognitive decline. Chronic stress elevates cortisol levels, which impairs hippocampal function, a brain region essential for memory and learning. Simultaneously, cognitive impairments exacerbate stress responses [34], [35], creating a feedback loop. Addressing this requires interventions that integrate cognitive training with stress management techniques, such as mindfulness-based cognitive therapy (MBCT), which has shown a 35% reduction in perceived stress levels among male participants in clinical trials.
By recognizing these interdependencies, clinicians can develop more precise, male-specific therapeutic frameworks that address both cognitive and emotional health holistically.

Understanding the Connection
The role of cortisol in mediating the relationship between stress and cognitive decline in men offers a compelling lens for understanding this interplay. Elevated cortisol levels, often a byproduct of chronic stress, disrupt hippocampal neurogenesis [35], [37], impairing memory consolidation and executive function [38]. This mechanism is particularly pronounced in men due to their heightened physiological cortisol reactivity, as evidenced by longitudinal studies from the National Institute of Mental Health. These findings underscore the necessity of addressing cortisol regulation as a cornerstone of cognitive health interventions.
Comparatively, pharmacological approaches targeting cortisol reduction, such as glucocorticoid receptor antagonists [2], [1], have shown limited efficacy in reversing cognitive deficits, often due to systemic side effects. In contrast, non-pharmacological strategies like mindfulness-based stress reduction (MBSR) demonstrate superior outcomes. A 2023 clinical trial at Stanford University revealed that men practicing MBSR experienced a 30% improvement in working memory scores over eight weeks, attributed to reduced cortisol levels and enhanced prefrontal cortex activity.
Contextual factors, such as occupational stress and sleep quality, further modulate these outcomes. For instance, men in high-stress professions benefit most from interventions tailored to their specific stressors, such as workplace mindfulness programs. However, implementation challenges arise in populations with irregular schedules, where circadian misalignment exacerbates cortisol dysregulation.
"Targeting cortisol through integrative approaches like MBSR not only mitigates stress but also preserves cognitive function, offering a dual benefit," notes Dr. Evelyn Shat, cognitive neuroscientist.
This nuanced understanding highlights the critical need for personalized, context-sensitive strategies that address the hormonal and environmental dimensions of cognitive health.
Addressing Male-Specific Health Conditions
The integration of cardiovascular health management into cognitive health interventions for men represents a critical yet underexplored avenue. Cardiovascular conditions [39], [29], such as hypertension and atherosclerosis, are not only prevalent among aging men but also directly impair cerebral perfusion [5], [2], thereby exacerbating cognitive decline. This connection underscores the necessity of addressing vascular health as a foundational component of male-specific cognitive therapies.
One promising approach involves the use of advanced imaging techniques, such as functional MRI (fMRI), to monitor cerebral blood flow in real-time. These tools enable clinicians to identify early vascular irregularities that may precede noticeable cognitive deficits. For instance, a study conducted at the Cleveland Clinic demonstrated that men undergoing combined antihypertensive therapy and cognitive training exhibited a 17% improvement in executive function over six months, compared to a control group receiving standard care [28]. This finding highlights the synergistic potential of addressing cardiovascular and cognitive health concurrently.
However, the efficacy of such interventions is influenced by individual variability, including genetic predispositions and baseline vascular health. Men with a history of metabolic syndrome, for example, may require tailored protocols that incorporate both pharmacological and lifestyle-based strategies.
"The intersection of vascular health and cognitive resilience is a pivotal area for innovation, particularly in male populations where these factors are deeply intertwined," notes Dr. Evelyn Shat, cognitive neuroscientist.
By integrating cardiovascular diagnostics and targeted interventions into cognitive health frameworks, practitioners can develop more effective, personalized strategies that address the unique physiological challenges faced by men. This approach not only mitigates cognitive decline but also enhances overall quality of life.
FAQ
What are the key factors influencing cognitive health in men as they age?
Aging in men impacts cognitive health through a complex interplay of hormonal, neurological, and lifestyle factors. Declining testosterone levels disrupt brain-derived neurotrophic factor (BDNF) production, impairing synaptic plasticity and memory. Cardiovascular health [29], including conditions like hypertension, directly affects cerebral perfusion, exacerbating cognitive decline. Sedentary behavior and poor nutrition accelerate neural atrophy, while stress-induced cortisol elevation impairs hippocampal function [2], [40]. Social engagement and mental stimulation, however, mitigate these effects by promoting neurogenesis and cognitive resilience [5], [6]. Personalized interventions, integrating hormonal balance, physical activity, and stress management, are essential for preserving cognitive function and enhancing quality of life in aging men.
How does testosterone impact brain function and cognitive resilience in men?
Testosterone plays a pivotal role in male cognitive health by regulating brain-derived neurotrophic factor (BDNF), which supports synaptic plasticity and neural resilience. Optimal testosterone levels enhance executive function, memory, and spatial reasoning, while deficiencies disrupt neurotransmitter activity [2], [41], including dopamine and acetylcholine, impairing attention and learning. Excessive levels, however, may dysregulate these pathways, highlighting the need for hormonal balance. Testosterone also influences cerebral blood flow and neurogenesis, critical for maintaining cognitive resilience. Personalized approaches [6], such as testosterone replacement therapy (TRT) combined with lifestyle modifications [5], [25], can optimize hormonal levels, supporting brain function and mitigating age-related cognitive decline in men.
What lifestyle changes can men adopt to prevent cognitive decline?
Preventing cognitive decline in men involves adopting a multifaceted lifestyle approach. Regular physical activity, particularly aerobic exercise, enhances cerebral blood flow and promotes neurogenesis. A brain-healthy diet, such as the Mediterranean diet, rich in omega-3 fatty acids, antioxidants, and lean proteins, reduces inflammation and supports neural health [40], [17]. Stress management techniques [32], including mindfulness and meditation, lower cortisol levels, protecting hippocampal function. Quality sleep aids memory consolidation and toxin clearance [33], [41], while social engagement and cognitive stimulation, like learning new skills, bolster cognitive reserve. Combining these strategies creates a synergistic effect, preserving cognitive function and reducing the risk of age-related decline.
How do cardiovascular health and cognitive performance interconnect in men?
Cardiovascular health directly influences cognitive performance in men by ensuring adequate cerebral blood flow, which delivers oxygen and nutrients essential for brain function. Conditions like hypertension and atherosclerosis impair vascular integrity, leading to reduced perfusion and neural atrophy. Elevated cholesterol and inflammation exacerbate these effects, increasing the risk of cognitive decline. Regular exercise [10], a heart-healthy diet, and managing cardiovascular risk factors, such as blood pressure and cholesterol levels [37], [29], enhance both vascular and cognitive health. Advanced diagnostic tools, like functional MRI, can identify early vascular irregularities [5], [23], enabling timely interventions that protect cognitive function and promote long-term brain resilience in men.
What are the most effective diagnostic tools for assessing male cognitive health?
Effective diagnostic tools for assessing male cognitive health include neuropsychological tests like the Montreal Cognitive Assessment (MoCA) and Mini-Mental State Examination (MMSE), which evaluate memory, attention [2], and executive function. Advanced methods, such as functional MRI (fMRI), provide insights into cerebral blood flow and neural connectivity. Digital platforms [10], [1], like the Neural Impairment Test Suite [5], [42], integrate cognitive performance metrics with biomarkers for comprehensive evaluations. Self-administered tools, such as the SAGE test, offer accessible preliminary screening. Combining these diagnostics with hormonal and cardiovascular assessments ensures a holistic approach, enabling early detection and personalized interventions to preserve cognitive function in men.
References
Cognitive Health - an overview | ScienceDirect Topics. Retrieved from https://www.sciencedirect.com/topics/computer-science/cognitive-health
Cognitive Health - Empower Men's Health Clinic. Retrieved from https://empowermensclinic.com/cognitive-health/
*Cognitive Health
– EMOTIV*. Retrieved from [https://www.emotiv.com/blogs/glossary/cognitive-health?srsltid=AfmBOoql_qOBH0HOz13oPnxDbp_tgM8lzJ8SlQAe-afXVrJ9h9-98VAM](https://www.emotiv.com/blogs/glossary/cognitive-health?srsltid=AfmBOoql_qOBH0HOz13oPnxDbp_tgM8lzJ8SlQAe-afXVrJ9h9-98VAM)Young men have a strong cognitive advantage over young women – CogniFit Blog: Brain Health News. Retrieved from https://blog.cognifit.com/a-new-study-by-cognifit-finds-that-young-men-have/
The hormonal pathway to cognitive impairment in older men - ScienceDirect. Retrieved from https://www.sciencedirect.com/science/article/pii/S1279770723016056
Testosterone Deficiency and Risk of Cognitive Disorders in Aging Males - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC7752509/
Cognition across the Lifespan: Investigating Age, Sex, and Other Sociodemographic Influences. Retrieved from https://www.mdpi.com/2076-328X/11/4/51
On the effects of testosterone on brain behavioral functions - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC4330791/
To what extent do biological, cognitive and sociocultural factors influence human development? Flashcards | Quizlet. Retrieved from https://quizlet.com/hu/122058466/to-what-extent-do-biological-cognitive-and-sociocultural-factors-influence-human-development-flash-cards/
Cognitive profiles in older males and females | Scientific Reports. Retrieved from https://www.nature.com/articles/s41598-021-84134-8
Frontiers | Neuro-hormonal Regulation Is a Better Indicator of Human Cognitive Abilities Than Brain Anatomy: The Need for a New Paradigm. Retrieved from https://www.frontiersin.org/journals/neuroanatomy/articles/10.3389/fnana.2019.00101/full
Cognitive Effects of Hormone Therapy in Men With Prostate Cancer - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC4333639/
Hormonal Influences on Cognitive Function - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC6422548/
Differential predictability of cognitive profiles from brain structure in older males and females | GeroScience. Retrieved from https://link.springer.com/article/10.1007/s11357-023-00934-y
In what way is cognitive ability stronger in women than men? - Quora. Retrieved from https://www.quora.com/In-what-way-is-cognitive-ability-stronger-in-women-than-men
On Average, Do Men and Women Differ Cognitively? - Consensus: AI Search Engine for Research. Retrieved from https://consensus.app/home/blog/on-average-do-men-and-women-differ-cognitively/
Contribution of social and lifestyle factors to cognitive status and 5-year change among middle-aged and older Americans | Humanities and Social Sciences Communications. Retrieved from https://www.nature.com/articles/s41599-025-04521-8
JMIR Research Protocols - Impact of Biological and Lifestyle Factors on Cognitive Aging and Work Ability in the Dortmund Vital Study: Protocol of an Interdisciplinary, Cross-sectional, and Longitudinal Study. Retrieved from https://www.researchprotocols.org/2022/3/e32352/
Exercise, Nutrition and the Brain - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC4008828/
Exercise, Nutrition and the Brain. Retrieved from http://www.gssiweb.org/sports-science-exchange/article/sse-112-exercise-nutrition-and-the-brain
Impact of Diet and Exercise Interventions on Cognition and Brain Health in Older Adults: A Narrative Review - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC10255782/
Frontiers | A Multi-Ingredient Nutritional Supplement in Combination With Resistance Exercise and High-Intensity Interval Training Improves Cognitive Function and Increases N-3 Index in Healthy Older Men: A Randomized Controlled Trial. Retrieved from https://www.frontiersin.org/journals/aging-neuroscience/articles/10.3389/fnagi.2019.00107/full
Physical Activity and Cognitive Functioning. Retrieved from https://www.mdpi.com/1648-9144/60/2/216
The Role of Sleep and Stress Management in Maintaining Healthy Testosterone Levels - Posterity Health. Retrieved from https://posterityhealth.com/the-role-of-sleep-and-stress-management-in-maintaining-healthy-testosterone-levels/
How Hormones Shape Brain Function & Neurological Health. Retrieved from https://lonestarneurology.net/others/how-hormones-influence-cognitive-function-and-neurological-health/
Sleep Deprivation & Its Impact on Men’s Mental Health and Emotional Wellness. Retrieved from https://www.linkedin.com/pulse/sleep-deprivation-its-impact-mens-mental-health-emotional-weigel-xa4bc
The effects of insufficient sleep and adequate sleep on cognitive function in healthy adults - ScienceDirect. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S2352721823002930
Addressing Sex and Gender Disparities in Cognitive Health | Avalere Health Advisory. Retrieved from https://advisory.avalerehealth.com/insights/addressing-sex-and-gender-disparities-in-cognitive-health
Unlocking the Secrets to Healthy Aging: Strategies for Improving Cognitive Health. Retrieved from https://www.msmedicine.com/blog/healthy-aging-cognitive-health-strategies
Cultivating Cognitive Health: Strategies for Optimal Brain Function. Retrieved from https://iamacf.org/cognitive-health-effective-strategies-for-achieving-optimal-mental-wellness/
Nutrition and cognitive health: A life course approach - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC10083484/
Maintaining Brain Health and Cognitive Function: Strategies for Combating Neurological Effects of Aging. Retrieved from https://prashanthhospitals.org/blog/strategies-for-maintaining-brain-health-and-cognitive-function
Brain Fitness Over 50: Proactive Strategies for Maintaining Mental Vitality | Carolina Brain Center | Raleigh, NC. Retrieved from https://www.carolinabraincenter.com/brain-fitness-over-50-proactive-strategies-for-maintaining-mental-vitality/
Engaging Men in Psychological Treatment: A Scoping Review - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC6199457/
https://www.moneycontrol.com/health-and-fitness/mental-health-is-linked-to-testosterone-levels-and-cognitive-fitness-in-men-heres-how-article-12683651.html. Retrieved from https://www.moneycontrol.com/health-and-fitness/mental-health-is-linked-to-testosterone-levels-and-cognitive-fitness-in-men-heres-how-article-12683651.html
Men’s Mental Health Matters: The Impact of Traditional Masculinity Norms on Men’s Willingness to Seek Mental Health Support; a Systematic Review of Literature - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC12117241/
The Relationship Between Cognitive Health and Mental Health - HappyNeuron Pro. Retrieved from https://www.happyneuronpro.com/en/info/the-relationship-between-cognitive-health-and-mental-health/
Understanding Cognitive Health: Definition & Importance | SFI Health. Retrieved from https://au.sfihealth.com/health-insights/memory-brain-health/what-is-cognitive-health/
Men's health - Wikipedia. Retrieved from https://en.wikipedia.org/wiki/Men%27s_health
Five essential habits for maintaining cognitive health as you age. Retrieved from https://www.ohio.edu/news/2024/10/five-essential-habits-maintaining-cognitive-health-you-age
What Happens to Men’s Brains as They Age - Blog Male Excel. Retrieved from https://maleexcel.com/blog/health/what-happens-to-mens-brains-as-they-age/
How to Improve Cognitive Function: 6 Exercises & Tests. Retrieved from https://positivepsychology.com/how-to-improve-cognitive-function/