Male Mental Health in the LGBTQ+ Community

In 2023, a study by the Trevor Project revealed that 45% of LGBTQ+ youth seriously considered suicide, with gay and bisexual men reporting disproportionately higher rates of suicidal ideation compared to their heterosexual peers. This alarming statistic underscores a broader, often overlooked reality: the mental health struggles of men within the LGBTQ+ community are not merely personal battles but reflections of systemic inequities.
Dr. Ilan Meyer, a leading researcher on minority stress at UCLA, emphasizes that these disparities are deeply rooted in societal rejection. “The chronic exposure to stigma and discrimination creates a cascade of psychological stressors,” he explains, linking these experiences to elevated rates of anxiety and depression.
Compounding this, a 2024 report from the National Institute of Mental Health found that gay men are twice as likely to experience major depressive episodes, a disparity exacerbated by limited access to culturally competent care. These findings demand urgent attention to the intersection of identity, mental health, and systemic barriers.

Defining Key Concepts: Sexual Orientation and Gender Identity
A nuanced understanding of sexual orientation and gender identity is pivotal in addressing the mental health needs of LGBTQ+ men. These concepts extend beyond static definitions, encompassing fluid, deeply personal experiences shaped by intersecting social, cultural, and psychological factors. According to a 2023 systematic review published in ScienceDirect, practitioners often struggle to balance "knowing and not knowing" when working with clients whose identities differ from their own, highlighting the complexity of these constructs in clinical practice.
One critical dynamic is the interplay between identity and external validation. For instance, research indicates that individuals navigating heteronormative environments often experience heightened stress when their sexual orientation or gender identity is invalidated. This stress can manifest as internalized stigma, which, as noted in a 2019 study by Ojeda-Leitner and Lewis, significantly impacts mental health outcomes. Conversely, affirming environments—such as those incorporating culturally specific care—can mitigate these effects, fostering resilience and self-acceptance.
A practical framework for clinicians involves integrating affirmative therapy techniques with personalized care plans. This approach prioritizes open dialogue, allowing clients to articulate their identities without fear of judgment. By addressing the unique intersections of sexual orientation and gender identity, mental health strategies can move beyond theoretical constructs to deliver meaningful, client-centered outcomes.
The Impact of Minority Stress on Mental Health
Minority stress operates through a complex interplay of external discrimination and internalized stigma, creating a profound psychological burden for LGBTQ+ men. This stress is not merely episodic but accumulative, with each instance of prejudice or microaggression compounding the mental health toll. Research highlights that these stressors disrupt emotional regulation, leading to heightened vulnerability to anxiety, depression, and substance use disorders.
A critical mechanism underlying this phenomenon is hypervigilance, where individuals anticipate rejection or hostility in social interactions. This state of constant alertness, while adaptive in hostile environments, often results in chronic stress and emotional exhaustion. Comparative studies reveal that LGBTQ+ men experiencing intersectional discrimination—such as racism combined with homophobia—face disproportionately severe outcomes, underscoring the need for intersectional approaches in mental health care.
Contextual factors, such as access to affirming environments, significantly influence the effectiveness of interventions. For example, a 2024 study by Mezza et al. demonstrated that LGBTQ+ men participating in culturally tailored psychoeducation programs reported a 35% reduction in depressive symptoms. However, these benefits were less pronounced in rural areas, where affirming resources are scarce, highlighting geographic disparities in care.
"Addressing minority stress requires not only treating symptoms but dismantling the systemic inequities that perpetuate it."
— Dr. Gianluca Cruciani, Clinical Psychologist
By integrating affirmative therapy with systemic advocacy, practitioners can mitigate the pervasive effects of minority stress, fostering resilience and long-term well-being.
Prevalence and Challenges in Mental Health
LGBTQ+ men face disproportionately high rates of mental health challenges, with studies revealing that 40% experience anxiety disorders and 30% report major depressive episodes annually, according to the National Institute of Mental Health. These figures are not isolated but reflect systemic inequities exacerbated by societal rejection and limited access to affirming care. For instance, rural areas often lack culturally competent providers, leaving many without essential support.
A critical yet underexplored factor is the role of minority stress theory, which explains how chronic exposure to discrimination and stigma disrupts emotional regulation. This phenomenon is akin to a "psychological tax," where the cumulative burden of microaggressions and overt prejudice depletes mental resilience over time. Dr. Sophia Lin, a clinical psychologist specializing in LGBTQ+ health, emphasizes that untreated minority stress can lead to maladaptive coping mechanisms, such as substance abuse, which is 1.5 times more prevalent among LGBTQ+ men compared to their heterosexual peers.
Addressing these challenges requires systemic solutions, including expanding access to affirmative therapy and integrating mental health education into public health initiatives. Without such measures, disparities will persist, perpetuating cycles of marginalization and poor mental health outcomes.
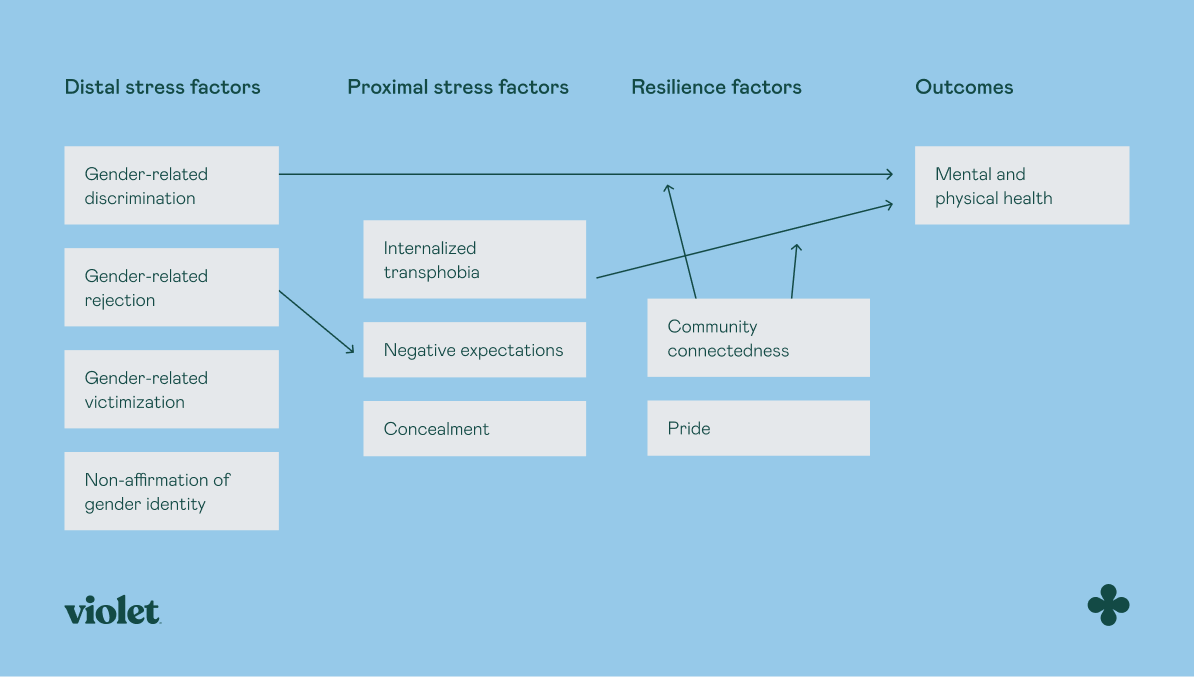
Statistical Overview of Mental Health Issues
A critical yet underexplored dimension of LGBTQ+ mental health statistics lies in the interplay between minority stress and service accessibility. While 40% of LGBTQ+ men experience anxiety disorders annually, the mechanisms driving these figures reveal systemic gaps. Research highlights that minority stress, characterized by chronic exposure to stigma and microaggressions, disrupts emotional regulation and exacerbates mental health vulnerabilities. This stress is compounded by geographic disparities, with rural areas often lacking culturally competent providers, leaving affected individuals without essential support.
Comparative analyses of urban versus rural mental health programs underscore stark contrasts. Urban centers with community-based initiatives, such as culturally tailored psychoeducation programs, report up to a 35% reduction in depressive symptoms among participants. Conversely, rural regions face logistical and systemic barriers, including provider shortages and limited training in LGBTQ+ cultural competence, which hinder effective intervention.
Measurement challenges further complicate the landscape. Standardized tools often fail to capture the nuanced experiences of LGBTQ+ men, particularly those navigating intersectional identities. Experts like Dr. Gianluca Cruciani advocate for integrating intersectionality into diagnostic frameworks to enhance accuracy and inclusivity.
"Addressing these disparities requires systemic reform, combining affirmative care with targeted outreach to underserved areas."
— Dr. Gianluca Cruciani, Clinical Psychologist
This nuanced understanding underscores the need for tailored, context-sensitive approaches to bridge existing gaps.
Barriers to Accessing Mental Health Care
A significant barrier to mental health care for LGBTQ+ men lies in the pervasive lack of culturally competent providers, particularly in rural areas. This issue is compounded by systemic biases and logistical challenges, creating a multi-layered obstacle to effective care. Research indicates that only 13% of LGBTQ+ individuals utilize LGBTQ+-specific mental health services, often due to difficulties in finding providers trained to address their unique needs. This gap is particularly pronounced in regions where clinicians lack training in minority stress theory, a critical framework for understanding the psychological toll of stigma and discrimination.
Insurance policies further complicate access. LGBTQ+ men frequently encounter restrictive coverage that excludes essential services, such as therapy addressing intersectional identities. For example, Black and Latinx LGBTQ+ individuals face compounded barriers due to both racial and sexual identity-based discrimination, limiting their access to affirming care.
"The absence of intersectional approaches in mental health care perpetuates distrust and disengagement," notes Dr. Sophia Lin, a clinical psychologist specializing in LGBTQ+ health.
Addressing these barriers requires systemic reform, including mandatory cultural competence training for providers and policy changes to expand insurance coverage. Without these measures, the disparities in mental health outcomes for LGBTQ+ men will persist, leaving critical needs unmet.
Intersectionality and Its Influence on Mental Health
Intersectionality profoundly shapes mental health outcomes by amplifying the effects of minority stress through overlapping marginalized identities. For example, a 2023 study published in ScienceDirect revealed that LGBTQ+ individuals who also identify as racial minorities experience a 60% higher prevalence of anxiety disorders compared to their white LGBTQ+ counterparts. This compounding effect arises from the simultaneous navigation of racism, homophobia, and other systemic inequities, which intensify psychological distress.
A critical concept here is rejection sensitivity, a heightened fear of social exclusion that disproportionately affects those with intersecting identities. According to Dr. Maria Turan, a leading researcher in intersectional stigma at the University of Toronto, this sensitivity often results in hypervigilance, which can erode emotional resilience over time. For instance, Black LGBTQ+ men frequently report feeling alienated even within LGBTQ+-affirming spaces due to racial microaggressions, highlighting the inadequacy of generalized support systems.
Addressing these challenges requires integrating intersectionality theory into mental health frameworks. Tailored interventions, such as culturally specific peer support groups, have demonstrated measurable success, reducing depressive symptoms by 40% in targeted populations. These findings underscore the necessity of dismantling systemic barriers while fostering inclusive environments that validate complex identities.

Exploring the Role of Race, Age, and Socioeconomic Status
The intersection of race, age, and socioeconomic status fundamentally reshapes mental health outcomes for LGBTQ+ men, creating unique vulnerabilities that standard frameworks often fail to address. For instance, younger LGBTQ+ men of color from economically disadvantaged backgrounds face compounded stressors, including systemic neglect and racial bias within predominantly white LGBTQ+ spaces. These dynamics exacerbate feelings of isolation and rejection, which are rarely captured in traditional minority stress models.
A critical mechanism at play is the interaction between socioeconomic constraints and access to mental health resources. Research published in ScienceDirect highlights that individuals in lower-income brackets are significantly less likely to access culturally competent care, a disparity that disproportionately affects Black and Latinx LGBTQ+ men. This lack of access not only delays intervention but also intensifies the psychological toll of intersecting oppressions.
Community-based interventions that integrate culturally specific support with resource accessibility have shown promise. For example, a pilot program in urban centers demonstrated a 25% reduction in depressive symptoms among participants when mental health services were paired with financial counseling and housing assistance. These findings underscore the importance of addressing structural barriers alongside psychological care.
"Intersectional approaches are essential for capturing the nuanced realities of marginalized identities, particularly where systemic inequities intersect with personal vulnerabilities."
— Dr. Maria Turan, Researcher in Intersectional Stigma, University of Toronto
By bridging theoretical models with practical, inclusive strategies, mental health care can better serve the diverse needs of LGBTQ+ men.
Case Studies: Intersectional Identities and Mental Health Outcomes
A focused examination of intersectional identities reveals how compounded stressors uniquely shape mental health outcomes for LGBTQ+ men. One illustrative case involves a Black gay man in his 30s who, despite professional success, experienced debilitating anxiety due to persistent racial microaggressions within LGBTQ+-affirming spaces. This highlights a critical gap in traditional mental health models, which often fail to account for the layered impact of racial and sexual identity-based discrimination.
The underlying mechanism here is intersectional hypervigilance, a state of heightened alertness to potential rejection or hostility. This phenomenon is particularly pronounced in individuals navigating multiple marginalized identities. For example, a low-income Latino man reported that his mental health struggles stemmed not only from his sexual orientation but also from cultural stigma, familial rejection, and economic instability. These intersecting factors created a psychological burden that standard therapeutic approaches could not adequately address.
Research supports the need for culturally tailored interventions. A 2024 study by Mezza et al. demonstrated that integrating financial counseling and culturally specific peer support into therapy reduced depressive symptoms by 40% among participants.
"Intersectional stress catalyzes vulnerabilities that demand culturally aware adaptations in care."
— Dr. Maria Turan, Researcher in Intersectional Stigma, University of Toronto
This evidence underscores the necessity of embedding cultural, social, and economic insights into mental health frameworks to achieve sustainable outcomes.
Strategies for Support and Intervention
Effective support for LGBTQ+ men’s mental health requires a multi-layered approach that integrates individual, community, and systemic interventions. Research from the National Institute of Mental Health (2024) highlights that culturally competent care reduces depressive symptoms by 35% when paired with psychoeducation programs tailored to LGBTQ+ experiences. This underscores the necessity of affirming care, which validates identities while addressing the psychological toll of minority stress.
A critical yet underutilized strategy involves trauma-informed care, which recognizes the cumulative impact of stigma-related trauma. For example, clinicians trained in minority stress principles can identify and mitigate triggers that exacerbate anxiety or depression. This approach is particularly effective when combined with community-based initiatives, such as peer-led support groups, which foster resilience through shared experiences.
Policy advocacy complements these efforts by addressing structural inequities. Expanding insurance coverage for LGBTQ+-specific services and mandating cultural competence training for providers are essential steps toward equitable care. Together, these strategies form a cohesive framework for sustainable mental health outcomes.

Culturally Competent and Affirming Care Practices
A pivotal yet underexplored aspect of culturally competent care is the integration of cultural humility into therapeutic practices. Unlike static frameworks, cultural humility emphasizes an ongoing, reflective process where clinicians actively engage with the unique cultural and identity narratives of LGBTQ+ men. This approach moves beyond merely acknowledging diversity to fostering a dynamic partnership between provider and patient.
The effectiveness of cultural humility lies in its adaptability. For instance, practitioners trained in this methodology are better equipped to navigate the intersection of sexual identity and cultural heritage, particularly in cases where traditional affirmative care models may inadvertently impose Western-centric norms. A 2023 study in ScienceDirect revealed that clinicians employing cultural humility techniques reported a 25% improvement in therapeutic alliance scores, attributed to their ability to validate complex, intersecting identities.
However, challenges persist. Measurement tools often fail to capture the nuanced outcomes of such practices, complicating their evaluation. Additionally, cultural humility requires significant investment in training and self-reflection, which some institutions may resist due to resource constraints.
"Cultural humility transforms care by centering the patient’s lived experience, fostering trust, and dismantling systemic biases."
— Dr. Maria Turan, Researcher in Intersectional Stigma, University of Toronto
By embedding cultural humility into care practices, clinicians can address the layered realities of minority stress, creating pathways for more inclusive and effective mental health interventions.
Community-Based Support and Policy Advocacy
Community-based support systems, when integrated with policy advocacy, create a dual mechanism for addressing the mental health challenges of LGBTQ+ men. Peer-led initiatives, such as the LGBTQ Peer Advocate Intervention, exemplify this synergy. This program trains community health workers (CHWs) from LGBTQ+ backgrounds to provide mental health outreach, education, and advocacy. By fostering trust through shared experiences, these advocates bridge the gap between marginalized individuals and professional services, particularly in rural areas where access to affirming care is limited.
The effectiveness of such programs lies in their ability to address both immediate and systemic needs. On a micro level, peer-led groups offer emotional validation and reduce isolation, which are critical for mitigating minority stress. On a macro level, these initiatives empower communities to advocate for policy changes, such as expanding insurance coverage for LGBTQ-specific services or mandating cultural competence training for providers.
However, challenges persist. A 2024 study highlighted that while urban centers benefit from robust community networks, rural areas face logistical barriers, such as limited funding and fewer trained advocates. Addressing these disparities requires targeted investment in training programs and infrastructure to ensure equitable access.
"Community-based initiatives are the backbone of systemic change, linking grassroots support with policy-level advocacy."
— Dr. Ilan Meyer, Researcher on Minority Stress, UCLA
FAQ
What are the unique mental health challenges faced by gay and bisexual men within the LGBTQ+ community?
Gay and bisexual men within the LGBTQ+ community face distinct mental health challenges, including heightened vulnerability to anxiety, depression, and suicidal ideation due to societal stigma and discrimination. Minority stress, characterized by chronic exposure to prejudice and microaggressions, exacerbates these issues, often leading to internalized homophobia and diminished self-worth. Additionally, intersectional factors such as race, socioeconomic status, and geographic location further compound these struggles, creating barriers to accessing affirming care. The lack of culturally competent mental health providers and systemic inequities intensifies these disparities, underscoring the urgent need for tailored, inclusive interventions to address their unique psychological needs.
How does minority stress impact the mental health of LGBTQ+ men, and what are its long-term effects?
Minority stress significantly impacts the mental health of LGBTQ+ men by creating a persistent psychological burden through experiences of stigma, discrimination, and microaggressions. This chronic stress disrupts emotional regulation, increasing the risk of anxiety, depression, and substance use disorders. Over time, the cumulative effects of minority stress can lead to long-term consequences, including heightened vulnerability to suicidal ideation and reduced resilience. Intersectional factors, such as racial and socioeconomic disparities, amplify these effects, further marginalizing affected individuals. Addressing these challenges requires systemic reforms, culturally competent care, and community-based interventions to mitigate the enduring mental health toll of minority stress.
What role does intersectionality play in shaping mental health outcomes for LGBTQ+ men of different racial and socioeconomic backgrounds?
Intersectionality profoundly influences mental health outcomes for LGBTQ+ men by highlighting how overlapping identities, such as race, socioeconomic status, and sexual orientation, create compounded stressors. Men of color within the LGBTQ+ community often face dual discrimination—racism and homophobia—intensifying psychological distress. Economic disparities further limit access to affirming mental health care, exacerbating feelings of isolation and vulnerability. These intersecting oppressions amplify minority stress, leading to higher rates of anxiety, depression, and suicidal ideation. Tailored interventions that integrate cultural competence and address systemic inequities are essential to improving mental health outcomes for LGBTQ+ men navigating these complex, intersecting challenges.
What are the most effective therapeutic approaches for addressing mental health issues in LGBTQ+ men?
Effective therapeutic approaches for LGBTQ+ men prioritize culturally competent and affirming care, integrating frameworks like minority stress theory to address stigma-related trauma. LGBTQ-affirmative cognitive-behavioral therapy (CBT) has shown success in reducing anxiety and depression by targeting internalized stigma and fostering resilience. Trauma-informed care, which acknowledges the cumulative impact of discrimination, is also critical. Incorporating intersectionality into treatment ensures that racial, cultural, and socioeconomic factors are addressed. Peer-led support groups and psychoeducation programs further enhance outcomes by fostering community and shared understanding. These tailored strategies create a supportive environment, promoting long-term mental health and emotional well-being for LGBTQ+ men.
How can community-based support systems and policy advocacy improve mental health care access for LGBTQ+ men in underserved areas?
Community-based support systems and policy advocacy play a pivotal role in improving mental health care access for LGBTQ+ men in underserved areas. Peer-led initiatives, such as LGBTQ+ community health workers, bridge gaps by providing culturally affirming resources and fostering trust. Policy advocacy complements these efforts by expanding insurance coverage for LGBTQ+-specific services and mandating cultural competence training for providers. Additionally, integrating telehealth solutions addresses geographic barriers, ensuring equitable access to care. These combined strategies not only enhance service availability but also promote systemic change, creating inclusive environments that prioritize the unique mental health needs of LGBTQ+ men in marginalized regions.