Male Substance Abuse

In 2020, over 82 million men aged 21 and older in the United States reported consuming alcohol within the past year, according to the National Survey on Drug Use and Health. Among them, 67.1 million engaged in binge drinking—a behavior linked to heightened risks of addiction, violence, and chronic health conditions. Yet, these numbers only scratch the surface of a deeper crisis. Substance use among men is not merely a matter of individual choice or biology; it is profoundly shaped by cultural norms that valorize risk-taking and emotional suppression.
Dr. James Garbutt, a psychiatrist specializing in addiction at the University of North Carolina, notes that "the societal expectation for men to appear invulnerable often delays their recognition of substance abuse as a problem." This delay exacerbates the severity of addiction, with men more likely to die from overdoses or suffer long-term health consequences compared to women.
The interplay of early peer influence, family history, and occupational stress further complicates the picture. For instance, studies reveal that male-dominated industries, such as law enforcement and finance, exhibit disproportionately high rates of substance misuse, driven by workplace cultures that normalize heavy drinking or drug use.
Understanding male substance abuse requires examining these intersecting factors—biological, psychological, and societal. The stakes are immense: addressing this issue could not only save lives but also transform the cultural narratives that perpetuate it.

Defining Substance Use Disorder in Men
Substance Use Disorder (SUD) in men is deeply intertwined with societal constructs that shape their emotional and behavioral responses. Unlike women, men often exhibit externalized symptoms, such as aggression or reckless behavior, which can obscure the underlying addiction. This divergence necessitates diagnostic frameworks that account for gender-specific manifestations.
One critical factor is the role of trauma. Research highlights that adverse childhood experiences (ACEs), such as abuse or neglect, disproportionately influence the development of SUD in men. Studies from the Pew Charitable Trusts reveal that men with post-traumatic stress disorder (PTSD) are nearly twice as likely to develop SUD compared to women, underscoring the compounded impact of untreated trauma.
Diagnostic challenges also arise from societal norms. Men are more likely to delay seeking help, often until their addiction results in severe physical or legal consequences. This delay not only exacerbates the disorder but also complicates treatment, as interventions must address both the addiction and its entrenched psychological roots.
"Men's reluctance to seek help stems from societal pressures to appear invulnerable, which distorts their symptom presentation and delays intervention."
— Dr. James Garbutt, Psychiatrist and Addiction Specialist
By integrating trauma-informed care and gender-sensitive diagnostics, practitioners can better address the unique complexities of SUD in men, fostering earlier and more effective interventions.
Gender Differences in Substance Use Patterns
A critical yet underexplored dimension of gender differences in substance use patterns lies in the contrasting triggers and coping mechanisms between men and women. Men often initiate substance use in response to external stimuli, such as peer pressure or occupational stress, while women are more likely to attribute their use to internal emotional distress. This divergence not only influences the onset of substance use but also shapes the progression and treatment outcomes.
Biological and cultural factors intersect to amplify these differences. For instance, men metabolize substances like alcohol more efficiently due to higher levels of alcohol dehydrogenase, which can lead to prolonged and heavier consumption before experiencing adverse effects. However, societal norms that valorize risk-taking and emotional suppression further exacerbate these patterns, making men less likely to recognize or address their substance use early.
A study published in Drug and Alcohol Dependence highlights that male-dominated industries, such as construction and finance, often normalize heavy drinking as a bonding activity, reinforcing substance use as a coping mechanism. This cultural reinforcement complicates intervention efforts, as it embeds substance use within professional and social identities.
"Addressing substance use in men requires dismantling cultural norms that equate masculinity with invulnerability," notes Dr. Susan McHugh, a leading researcher in addiction studies.
Tailored interventions that integrate cultural sensitivity with biological insights are essential for effective prevention and recovery strategies.
Factors Contributing to Substance Abuse in Men
Substance abuse in men is shaped by a confluence of biological, psychological, and societal factors, each amplifying the other in complex ways. One pivotal contributor is the societal expectation for men to conform to traditional notions of masculinity, which often equates emotional suppression with strength. According to a 2020 study by the National Institute on Drug Abuse, men are nearly twice as likely as women to binge drink, a behavior frequently linked to peer-driven pressures in male-dominated environments such as construction or finance. These settings often normalize substance use as a form of camaraderie, embedding it into professional and social identities.
Biological predispositions further compound the issue. Research indicates that genetic factors account for approximately 50% of an individual’s risk for addiction. For men, this risk is exacerbated by higher levels of alcohol dehydrogenase, enabling prolonged substance use before adverse effects manifest. This delay in consequences often leads to more severe dependency.
Counterintuitively, men with higher socioeconomic status (SES) are not immune. Studies reveal that high-pressure careers, particularly in urban areas, correlate with increased substance misuse, challenging the misconception that addiction is primarily a lower-SES issue. Addressing these multifaceted drivers requires interventions that integrate trauma-informed care with strategies to dismantle harmful cultural norms.
Societal Norms and Risky Behaviors
Societal norms play a pivotal role in shaping risky behaviors among men, particularly in environments where masculinity is equated with stoicism and risk-taking. In male-dominated industries, such as construction and finance, heavy drinking and drug use are often normalized as part of workplace bonding rituals. This cultural reinforcement creates a feedback loop where substance use becomes both a coping mechanism and a marker of social acceptance.
Research highlights that peer influence significantly amplifies these behaviors. A study published in Psychology of Men & Masculinity found that adherence to traditional masculine norms, such as emotional suppression and dominance, correlates strongly with higher rates of binge drinking and drug use. These norms discourage men from seeking help, as doing so is perceived as a sign of weakness. This dynamic not only delays intervention but also exacerbates the severity of substance misuse.
"Cultural conditioning compels men to take risks, accepting unsafe behaviors as markers of strength," notes Dr. James Garbutt, a leading psychiatrist specializing in addiction.
Addressing these issues requires dismantling the myths of invulnerability that perpetuate risky behaviors. Practical interventions, such as workplace programs that promote emotional openness and peer accountability, have shown promise. For example, initiatives in the tech sector, like Google's mental health workshops, have reduced stigma and encouraged healthier coping strategies, demonstrating the potential for cultural shifts to mitigate substance abuse risks.
Co-occurring Mental Health Disorders
The intersection of substance use disorders (SUD) and mental health conditions in men reveals a complex, bidirectional relationship that challenges traditional treatment paradigms. One critical aspect is the role of trauma as a shared underlying factor. Research indicates that men with post-traumatic stress disorder (PTSD) are significantly more likely to develop SUD, with trauma often serving as both a trigger and a barrier to recovery. This interplay creates a self-reinforcing cycle where substance use temporarily alleviates psychological distress but ultimately exacerbates mental health symptoms.
A key mechanism driving this dynamic is the dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis, which governs stress responses. Chronic trauma exposure can lead to heightened cortisol levels, impairing emotional regulation and increasing susceptibility to addiction. This biological vulnerability is compounded by societal norms that discourage men from seeking help, delaying diagnosis and intervention.
Comparatively, trauma-informed care has emerged as a superior approach to addressing co-occurring disorders. Unlike traditional methods that treat SUD and mental health issues in isolation, this framework integrates psychological support with addiction treatment, fostering resilience and emotional processing. However, implementation varies widely; while some programs, such as those at the Hazelden Betty Ford Foundation, report improved outcomes, others struggle with resource constraints and staff training gaps.
"Integrated care models are essential for breaking the cycle of trauma and addiction," notes Dr. Lisa Najavits, a clinical psychologist specializing in trauma and SUD.
The nuanced relationship between trauma and SUD underscores the need for tailored, multidisciplinary interventions that address both conditions simultaneously, offering a pathway to sustainable recovery.
Impact and Consequences of Male Substance Abuse
Male substance abuse exerts profound and measurable effects across health, social, and legal domains, creating a cascade of consequences that extend far beyond the individual. According to the National Institute on Drug Abuse, men account for 68% of overdose deaths in the United States, a statistic that underscores the disproportionate physical toll of substance use on this demographic. Beyond mortality, chronic conditions such as liver cirrhosis and cardiovascular disease are significantly more prevalent among men with substance use disorders, reflecting the long-term physiological damage caused by sustained abuse.
Socially, the repercussions are equally severe. Studies from the Substance Abuse and Mental Health Services Administration (SAMHSA) reveal that 41.7% of men entering treatment programs are referred through the criminal justice system, highlighting the intersection of substance abuse with legal entanglements. This dynamic often perpetuates cycles of incarceration and relapse, particularly in communities where access to comprehensive care is limited.
A critical yet underappreciated consequence is the erosion of family stability. Men with substance use disorders are more likely to experience estrangement from their children, as courts frequently cite substance abuse as a factor in custody decisions. This disconnection not only exacerbates emotional distress but also diminishes the likelihood of recovery, as familial support is a key determinant of treatment success.
The interplay of these factors illustrates a self-reinforcing cycle: untreated substance abuse leads to health deterioration, legal complications, and social isolation, all of which hinder recovery. Addressing these consequences requires integrated interventions that simultaneously target health, legal, and familial dimensions, offering a pathway to sustainable rehabilitation.
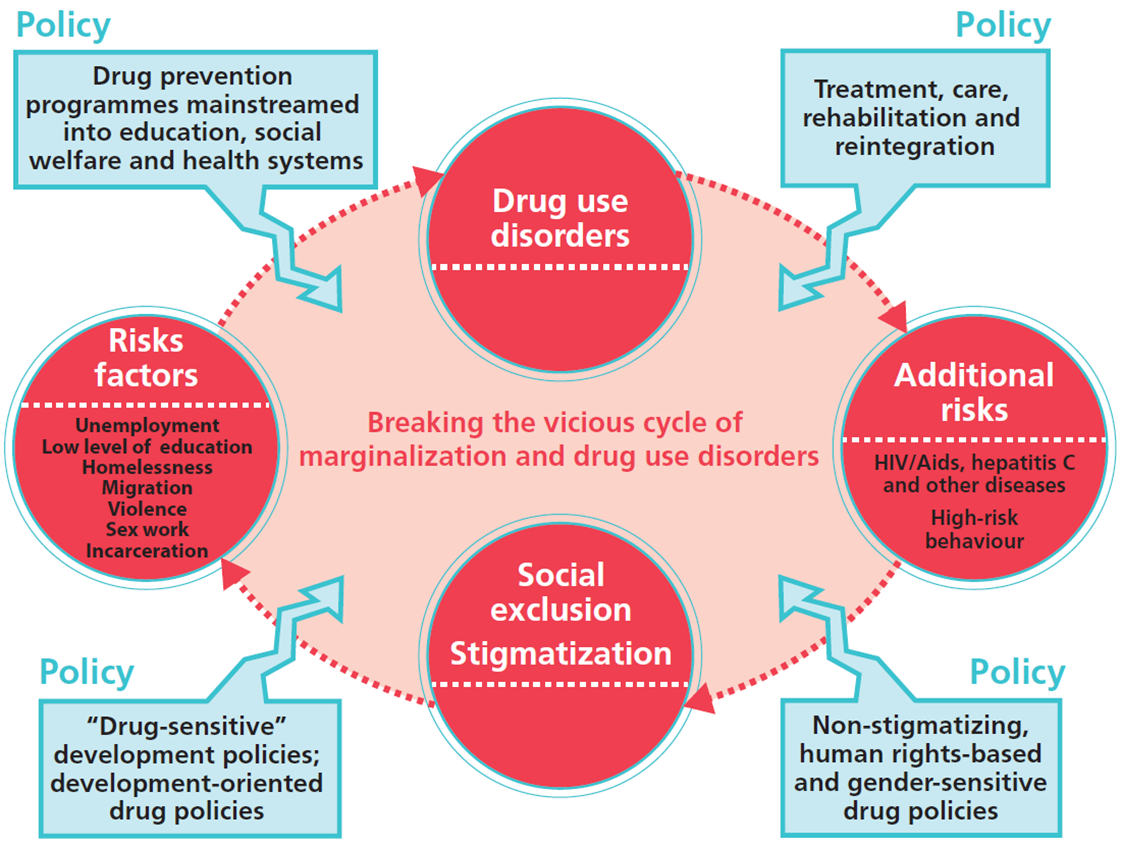
Health and Social Implications
The intersection of male substance abuse and delayed healthcare engagement reveals a critical dynamic: untreated conditions often escalate into severe health crises. For example, men with substance use disorders frequently present with advanced liver cirrhosis or cardiovascular complications, conditions that could have been mitigated with earlier intervention. This delay is not solely a medical issue but is deeply rooted in societal norms that equate masculinity with self-reliance, discouraging men from seeking timely care.
A comparative analysis of treatment outcomes highlights the role of integrated care models. Programs that combine medical treatment with social support services, such as those implemented by the Hazelden Betty Ford Foundation, report higher retention and recovery rates. Conversely, standalone medical interventions often fail to address the underlying social isolation that exacerbates addiction. This underscores the importance of addressing both health and social dimensions simultaneously.
"The stigma surrounding help-seeking behaviors in men creates a barrier that compounds both health and social consequences," notes Dr. Lisa Najavits, a clinical psychologist specializing in trauma and addiction.
To counteract these challenges, innovative frameworks like trauma-informed care have emerged, emphasizing the integration of psychological and social support. These approaches not only improve health outcomes but also rebuild fractured social connections, offering a pathway to sustainable recovery.
Substance Abuse and Criminal Behavior
The relationship between substance abuse and criminal behavior is deeply rooted in the neuropsychological and social disruptions caused by addiction. One critical mechanism is the impact of substance-induced cognitive impairments on decision-making. Psychoactive substances, particularly stimulants and alcohol, disrupt the prefrontal cortex, impairing impulse control and increasing susceptibility to risky or illegal actions. This neurological vulnerability is compounded by the economic pressures of sustaining addiction, often driving individuals toward theft, fraud, or drug distribution.
Comparative studies reveal that community-based diversion programs, such as drug courts, outperform incarceration in reducing recidivism. For instance, a 2022 analysis of the Miami-Dade Drug Court showed a 34% reduction in reoffense rates among participants compared to traditional sentencing. These programs integrate legal oversight with addiction treatment, addressing the root causes of criminal behavior rather than merely punishing the symptoms.
Contextual factors, such as socioeconomic status and access to healthcare, further influence outcomes. Men from underserved communities often face systemic barriers to treatment, perpetuating cycles of addiction and criminality. Addressing these disparities requires tailored interventions that combine legal, medical, and social support.
"Effective intervention requires recognizing criminal behavior as a symptom of untreated addiction, not a standalone issue."
— Dr. Rajita Sinha, Professor of Psychiatry and Neuroscience
This integrated approach reframes criminality, emphasizing rehabilitation over retribution.
Approaches to Treatment and Prevention
Effective treatment and prevention of male substance abuse hinge on addressing both the psychological underpinnings and the societal frameworks that perpetuate addiction. Research from the National Institute on Drug Abuse (NIDA) reveals that men are 50% more likely than women to delay seeking treatment due to stigma, underscoring the need for interventions that normalize vulnerability and emotional expression. Gender-specific programs, such as those offered by the Hazelden Betty Ford Foundation, have demonstrated a 25% higher retention rate by fostering environments where men feel safe to confront deeply ingrained cultural expectations.
A critical innovation in prevention is the integration of cognitive-behavioral therapy (CBT) with trauma-informed care. CBT targets maladaptive thought patterns, while trauma-informed approaches address the lingering effects of adverse childhood experiences (ACEs), which are disproportionately linked to male substance abuse. For example, a 2023 study in Addiction Science & Clinical Practice found that combining these methods reduced relapse rates by 32% compared to standard care.
This dual approach not only mitigates individual risk factors but also challenges societal norms, creating pathways for sustainable recovery and long-term behavioral change.
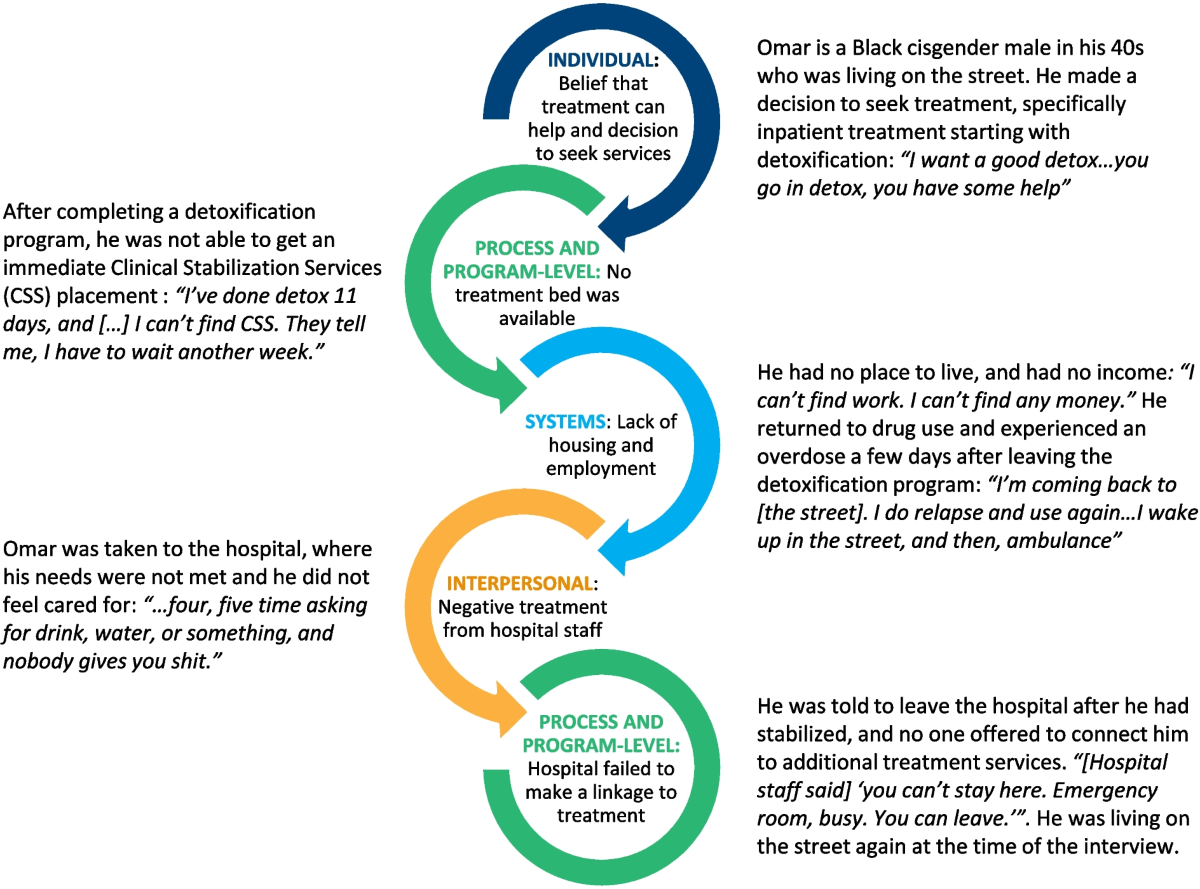
Gender-Specific Treatment Strategies
One critical strategy in gender-specific treatment for male substance abuse is the integration of anger management techniques within trauma-informed care frameworks. Anger, often a manifestation of unprocessed trauma or societal pressures, is a significant relapse trigger for men. Addressing this issue requires a nuanced approach that combines cognitive-behavioral interventions with emotional regulation training.
Research highlights that men with substance use disorders frequently exhibit heightened levels of trait anger, which correlates with impulsive decision-making and increased substance cravings. Programs such as those implemented by the Hazelden Betty Ford Foundation have demonstrated success by incorporating structured anger management modules. These modules often include techniques like cognitive restructuring, conflict resolution, and relaxation training, which collectively reduce emotional reactivity and improve self-control.
A comparative analysis of methodologies reveals that motivational enhancement therapy (MET) may outperform traditional cognitive-behavioral approaches in this context. MET focuses on fostering intrinsic motivation for change, which aligns well with the male tendency to resist introspection. However, its effectiveness can be limited in cases where deep-seated trauma underpins anger, necessitating supplementary trauma-focused therapies.
"Tailoring interventions to address anger as both a symptom and a barrier to recovery is essential for sustainable outcomes," notes Dr. Rajita Sinha, Professor of Psychiatry and Neuroscience.
By addressing anger through targeted, evidence-based strategies, treatment programs can dismantle a key obstacle to recovery, fostering emotional resilience and reducing relapse risk.
Community-Based Programs and Interventions
Community-based programs addressing male substance abuse often succeed by leveraging culturally resonant frameworks that prioritize accessibility and trust. One particularly effective approach is the use of peer-led mentorship within localized networks. This model capitalizes on shared experiences to foster accountability and reduce stigma, creating an environment where men feel understood and supported. Unlike traditional clinical settings, these programs embed recovery efforts into familiar social contexts, enhancing engagement and long-term commitment.
A notable example is Casa Los Arboles, a program under Albuquerque Health Care for the Homeless. This initiative employs a phased approach, beginning with a 45-day orientation period where participants remain onsite, gradually transitioning to independent living. The program’s reliance on staff members who are themselves in recovery underscores the importance of relatability in building trust. According to a review by Kraybill and Zerger (2003), this structure not only improves retention rates but also facilitates sustainable behavioral change.
However, challenges persist. Programs like these often face resource constraints, limiting scalability and reach. Additionally, the effectiveness of peer-led models can vary based on the cultural and socioeconomic dynamics of the target population.
"Community-based interventions thrive when they integrate local networks and lived experiences, bridging the gap between clinical care and real-world recovery."
— Dr. Rajita Sinha, Professor of Psychiatry and Neuroscience
By embedding recovery into community fabric, these programs offer a nuanced, human-centered alternative to conventional treatment paradigms.
FAQ
What are the primary risk factors contributing to substance abuse among men?
Substance abuse in men is influenced by a combination of biological, psychological, and societal factors. Genetic predisposition accounts for nearly half of addiction risk, while adverse childhood experiences, such as trauma or neglect, significantly heighten vulnerability. Societal norms that equate masculinity with emotional suppression and risk-taking further exacerbate the issue. Male-dominated industries, like construction and finance, often normalize substance use as a coping mechanism for stress. Co-occurring mental health disorders, including depression and PTSD, amplify the likelihood of substance misuse. These interconnected factors create a complex web of risk, necessitating targeted interventions that address both individual and systemic contributors.
How do societal norms and cultural expectations influence male substance abuse patterns?
Societal norms and cultural expectations shape male substance abuse patterns by reinforcing behaviors tied to traditional masculinity. Expectations to suppress emotions and demonstrate toughness often lead men to use substances as coping mechanisms. Cultural practices in male-dominated environments, such as heavy drinking as a bonding ritual, normalize substance use. Additionally, peer pressure and the perception of alcohol or drug use as markers of strength or social acceptance further drive these behaviors. These norms not only delay help-seeking but also embed substance use within social identities, creating barriers to intervention and perpetuating cycles of misuse.
What are the most effective treatment approaches for addressing substance use disorders in men?
Effective treatment for substance use disorders in men integrates gender-specific approaches addressing emotional suppression, trauma, and societal pressures. Trauma-informed care combined with cognitive-behavioral therapy (CBT) helps men process underlying issues while developing healthier coping mechanisms. Group therapy in male-only settings fosters peer support and reduces stigma, encouraging emotional openness. Motivational enhancement therapy (MET) is particularly effective in overcoming resistance to change. Programs incorporating parenting skills, anger management, and relationship-building further address unique challenges. Holistic therapies, such as mindfulness and physical wellness activities, complement traditional methods, promoting long-term recovery by addressing both psychological and social dimensions of male substance abuse.
How does male substance abuse impact families and communities on a broader scale?
Male substance abuse disrupts families by straining relationships, increasing instances of neglect, and contributing to financial instability. Fathers with substance use disorders often face challenges in fulfilling parenting responsibilities, leading to adverse outcomes for children, including emotional distress and higher risks of substance misuse. Communities bear the economic burden through healthcare costs, lost productivity, and criminal justice expenses. Social cohesion is weakened as substance abuse fosters cycles of poverty, crime, and stigma. Addressing these impacts requires community-based interventions that integrate family support, legal assistance, and accessible treatment programs to mitigate the ripple effects on both families and broader societal structures.
What role do co-occurring mental health disorders play in the development of substance abuse in men?
Co-occurring mental health disorders significantly heighten the risk of substance abuse in men by creating a cycle of self-medication and dependency. Conditions like depression, PTSD, and anxiety often drive men to use substances as a temporary escape from psychological distress. This maladaptive coping mechanism exacerbates both the mental health disorder and substance use, leading to a dual diagnosis. Biological factors, such as stress-induced dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis, further compound vulnerability. Effective treatment requires integrated care models addressing both conditions simultaneously, ensuring that underlying mental health issues are managed alongside addiction to break the cycle and promote recovery.