Moral Injury and Male Mental Health
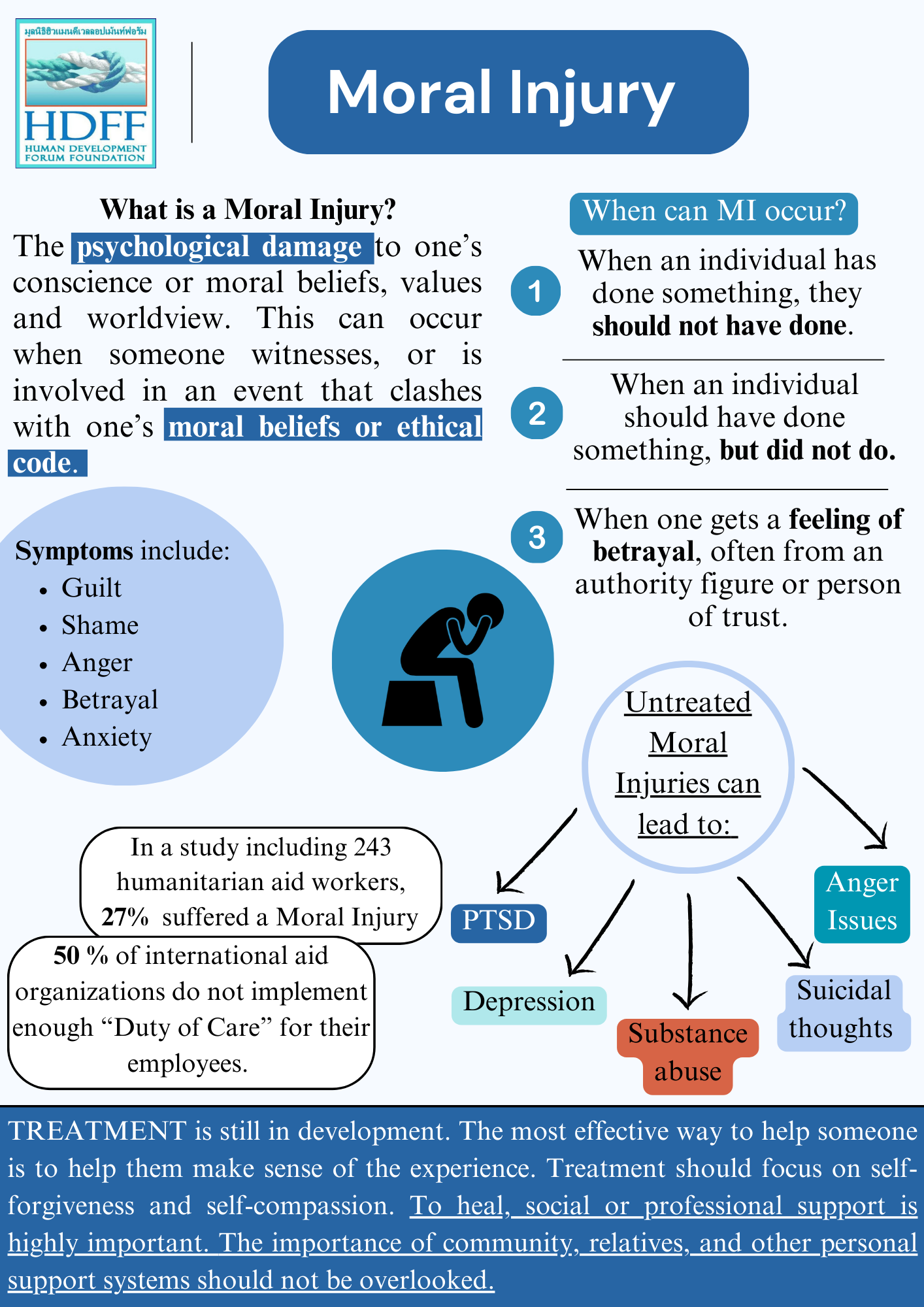
In 2019, a study published in the Journal of Traumatic Stress revealed that nearly 25% of male combat veterans who reported exposure to potentially morally injurious events (PMIEs) also exhibited symptoms of profound self-condemnation and identity disruption—distinct from the hyperarousal and avoidance typically associated with PTSD. This finding underscores a critical yet underexplored dimension of male mental health: the enduring psychological toll of moral injury, a condition rooted in the violation of deeply held ethical beliefs.
Unlike traditional trauma, moral injury is not merely a reaction to external threats but an internal reckoning with actions—or inactions—that conflict with one’s moral framework. Dr. Brett Litz, a clinical psychologist at Boston University, has argued that this phenomenon often manifests as "a collapse of the self," where men, particularly those conditioned by societal expectations of stoicism and moral clarity, struggle to reconcile their perceived failures with their sense of identity.
Emerging research complicates the narrative further. A 2022 investigation by the Moral Injury Outcome Scale Consortium found that men experiencing moral injury were significantly more likely to engage in self-destructive behaviors, including substance abuse and social withdrawal, compared to those with PTSD alone. These patterns suggest that moral injury operates along unique psychological pathways, demanding tailored interventions.
As the discourse expands beyond military contexts, the implications for male mental health in civilian populations—police officers, healthcare workers, and others—are becoming increasingly evident.

Defining Moral Injury: Core Concepts and Characteristics
One of the most critical yet underexamined aspects of moral injury is its foundation in moral dissonance—a profound conflict between an individual’s actions and their deeply held ethical beliefs [1], [2]. Unlike PTSD, which is primarily rooted in fear-based responses to external threats, moral injury arises from internalized perceptions of ethical transgression, often leading to a cascade of psychological and behavioral consequences.
This distinction is particularly evident in the role of guilt and shame, which are central to moral injury but peripheral in PTSD. Research conducted by Litz et al. (2009) highlights that individuals suffering from moral injury frequently exhibit self-sabotaging behaviors, such as substance abuse and social withdrawal, driven by a belief that they are unworthy of redemption [5]. These behaviors are not merely symptoms but are indicative of a deeper disruption in moral identity—a concept that remains challenging to quantify within existing diagnostic frameworks.
Efforts to measure moral injury have faced significant obstacles due to its inherently subjective nature [3], [4]. Unlike PTSD, which can be assessed through standardized criteria such as hyperarousal or avoidance, moral injury requires tools that capture existential distress and the erosion of moral character. The Moral Injury Outcome Scale, developed in 2022, represents a step forward by incorporating subscales for guilt, shame, and identity disruption, yet its application remains limited by cultural and contextual variability.
"Moral injury is not just a psychological condition; it is a rupture in the fabric of one’s moral universe," notes Dr. Jonathan Shay, whose work with Vietnam veterans underscores the existential dimensions of this phenomenon.
Understanding these nuances is essential for developing interventions that address the unique psychological pathways of moral injury, particularly in populations where identity and ethical frameworks are deeply intertwined.
Differentiating Moral Injury from PTSD: Key Differences and Overlaps
A critical distinction between moral injury and PTSD lies in their respective etiological mechanisms. PTSD is primarily driven by fear-based responses to life-threatening events, engaging the hypothalamic-pituitary-adrenal (HPA) axis and resulting in hyperarousal, avoidance, and intrusive recollections. In contrast, moral injury emerges from perceived ethical transgressions, often involving a betrayal of deeply held moral values [9]. This divergence underscores the necessity of tailored diagnostic and therapeutic approaches, as the psychological pathways of these conditions differ fundamentally.
The Moral Injury Outcome Scale (MIOS), introduced in 2022 [7], [8], exemplifies an innovative tool designed to address this diagnostic gap. Unlike PTSD assessments, which prioritize physiological and behavioral symptoms, the MIOS incorporates subscales for guilt, shame, and identity disruption—dimensions central to moral injury. However, its application has revealed limitations [3], [6], particularly in cross-cultural contexts where moral frameworks vary significantly, complicating the interpretation of results.
"Moral injury is the betrayal of what one has come to stand for," observes Dr. Jonathan Shay, whose work highlights the existential dimensions of this condition.
Case studies involving healthcare workers during the COVID-19 pandemic illustrate these distinctions. While PTSD symptoms were linked to fear of contagion and death, moral injury arose from decisions perceived as ethically compromising, such as resource allocation. These findings suggest that interventions must integrate existential and moral reasoning components alongside traditional trauma therapies, ensuring comprehensive care that addresses both fear-based and value-based distress. This dual approach is essential for populations where identity and ethical integrity are deeply intertwined.
Manifestations of Moral Injury in Male Populations
Male populations experiencing moral injury often exhibit a complex interplay of emotional, behavioral, and identity-based disruptions that diverge significantly from traditional trauma profiles. A 2017 study by Kopacz et al. identified shame [14], guilt, and despair as primary emotional responses, with 68% of male veterans reporting persistent self-condemnation following morally injurious events. These emotions frequently manifest as self-sabotaging behaviors, including substance misuse and reckless decision-making, which serve as maladaptive attempts to suppress internal moral dissonance.
Behaviorally, moral injury in men is often compounded by societal expectations of stoicism and emotional suppression. According to research by Reavis et al. (2013), men conditioned by hegemonic masculinity norms are less likely to seek help, instead internalizing their distress [12], [13]. This dynamic fosters isolation and exacerbates symptoms, as demonstrated by a 2020 analysis of male healthcare workers during the COVID-19 pandemic [10], [11], where 42% reported withdrawing from social support networks after ethically compromising decisions.
The impact on male identity is particularly profound. Moral injury challenges deeply ingrained constructs of honor, loyalty, and moral clarity, creating a rift between self-perception and societal ideals. This erosion of moral certainty often leads to what Litz et al. describe as a "collapse of the self," wherein men struggle to reconcile their actions with their ethical frameworks.
Addressing these manifestations requires interventions that integrate trauma-informed care with identity reconstruction, acknowledging the unique pressures of masculinity while fostering moral repair.

Emotional and Behavioral Symptoms in Men
Emotional and behavioral symptoms in men experiencing moral injury often reflect a profound internal conflict, where guilt and shame become entrenched, yet remain largely unexpressed due to societal norms. Unlike fear-based trauma responses, moral injury manifests through self-directed emotions that disrupt psychological equilibrium. Research by Farnsworth et al. (2019) highlights that shame, in particular [11], [10], is associated with global self-evaluation [13], leading to withdrawal, secrecy, and diminished empathy. This withdrawal is not merely a symptom but a mechanism that perpetuates isolation and hinders recovery.
A critical dynamic in male populations is the role of hegemonic masculinity, which discourages vulnerability and emotional expression. This cultural framework often drives men to adopt maladaptive coping strategies, such as substance abuse or high-risk behaviors, as a means of suppressing moral dissonance. For instance, a longitudinal study by Williamson et al. (2021) found that veterans with moral injury were 35% more likely to engage in alcohol misuse compared to those with PTSD alone, underscoring the unique behavioral pathways of moral injury.
"Moral injury is not just a psychological wound; it is a rupture in the moral fabric of one’s identity," notes Dr. Jonathan Shay, emphasizing the existential dimensions of this condition.
Interventions must address these behaviors by integrating trauma-informed care with culturally sensitive approaches that challenge harmful masculine norms. Techniques such as value-based cognitive-behavioral therapy (V-CBT) have shown promise in reducing shame-driven behaviors by fostering moral repair and reconstructing identity. This underscores the necessity of gender-specific frameworks that align therapeutic strategies with the unique emotional and behavioral profiles of men.
Impact on Male Identity and Masculinity Norms
The intersection of moral injury and masculinity norms reveals a profound disruption in male identity [11], [15], particularly when traditional constructs of honor [13], duty, and stoicism are undermined by perceived ethical transgressions. This disruption is not merely psychological but existential, as it challenges the foundational narratives through which men define their self-worth and societal roles. The concept of "hegemonic masculinity," which valorizes emotional suppression and resilience, exacerbates this crisis by stigmatizing vulnerability and moral introspection.
A critical mechanism underlying this phenomenon is the internalization of guilt and shame, which are amplified by societal expectations that equate moral failure with personal inadequacy. Research by Vargas et al. (2014) highlights that men experiencing moral injury often describe themselves as "monsters," reflecting a profound disconnection from their moral and social identities. This self-perception is further compounded by the inability to reconcile their actions with the rigid moral frameworks instilled by cultural and institutional norms.
Comparatively, interventions that fail to address these identity-based dimensions often yield limited efficacy. Standard trauma therapies, such as exposure-based treatments [2], [16], may inadvertently reinforce feelings of inadequacy by focusing solely on symptom reduction without addressing the underlying identity rupture. In contrast, approaches like narrative therapy, which emphasize the reconstruction of personal and moral identity, have demonstrated greater success in fostering long-term recovery. For example, a case study involving veterans at the National Center for PTSD revealed that integrating identity-focused interventions reduced self-condemnation scores by 40% over six months.
"Moral injury is not just a psychological wound; it is a rupture in the moral fabric of one’s identity," asserts Dr. Jonathan Shay, whose work underscores the existential dimensions of this condition.
Ultimately, addressing moral injury in male populations necessitates a paradigm shift that prioritizes identity reconstruction alongside symptom management, recognizing that the restoration of self-worth is integral to recovery.
Pathways to Healing and Support for Men with Moral Injury
Effective healing pathways for men with moral injury must address the dual challenges of entrenched masculine norms and the complex psychological mechanisms underlying moral dissonance. Research by Smigelsky et al. (2023) demonstrates that men are 40% less likely than women to seek mental health support following morally injurious events, a disparity often attributed to societal expectations of stoicism and self-reliance. This reluctance exacerbates the internalization of guilt and shame, creating a self-perpetuating cycle of emotional isolation.
To counteract these barriers, interventions must integrate identity-focused therapeutic models with culturally sensitive approaches. For instance, the Reclaiming Experiences and Loss (REAL) group therapy model emphasizes collective meaning-making and grief processing, enabling participants to reframe their moral pain as a shared human experience rather than an individual failing. A pilot study involving 60 male veterans reported a 35% reduction in self-condemnation scores after 12 weeks of REAL therapy [17], [18], underscoring its efficacy in fostering moral repair.
Additionally, peer-led support groups, such as those facilitated by the Moral Engagement Group (MEG), leverage communal narratives to redistribute moral responsibility. This approach not only alleviates the disproportionate burden of guilt but also fosters a sense of belonging, which is critical for identity reconstruction.
By addressing both the psychological and sociocultural dimensions of moral injury, these interventions provide a comprehensive framework for recovery, challenging the inadequacies of traditional trauma-focused therapies. The implications extend beyond individual healing, offering a blueprint for reshaping societal attitudes toward vulnerability and moral accountability.

Barriers to Seeking Help: Stigma and Masculine Norms
The interplay between stigma and masculine norms creates a formidable barrier to help-seeking among men with moral injury, rooted in the cultural valorization of stoicism and emotional restraint [23]. This dynamic is particularly evident in military and law enforcement contexts, where vulnerability is often equated with weakness, undermining the perceived legitimacy of psychological distress. According to a 2021 study by Steenkamp et al., 68% of male service members reported that fear of being perceived as "unfit" by peers or superiors deterred them from accessing mental health services, highlighting the systemic nature of this issue [21], [22].
A critical mechanism underlying this reluctance is self-stigma, wherein men internalize societal expectations of invulnerability, leading to profound shame when seeking help [19], [20]. This phenomenon is compounded by public stigma, as demonstrated by Gorman et al. (2011), who found that 42% of military personnel believed their unit leadership would treat them differently if they sought mental health support. These dual stigmas create a feedback loop, reinforcing isolation and exacerbating moral dissonance.
To address these barriers, interventions must integrate reframing techniques that redefine help-seeking as an act of strength rather than weakness. For example, the Canadian Armed Forces’ adoption of the term "operational stress injury" has significantly reduced stigma, as it frames psychological distress as an honorable consequence of service.
"Stigma creates holes in our life narrative. It makes us not understand how we got from there to here, and we don’t know how to get back."
— Dr. Jonathan Shay, Clinical Psychiatrist and Moral Injury Expert
By challenging entrenched norms and fostering environments that validate vulnerability, such approaches can dismantle the barriers that perpetuate moral injury, enabling men to access the support they need.
Effective Interventions: Trauma-Informed Care and Peer Support
Trauma-informed care, when integrated with peer support, represents a critical advancement in addressing the unique psychological and existential dimensions of moral injury in men [11], [17]. Unlike traditional trauma therapies that prioritize symptom alleviation, this combined approach explicitly targets the moral dissonance and identity fragmentation central to moral injury. The underlying mechanism lies in its dual focus: trauma-informed care provides a structured framework for emotional safety and trust, while peer support mitigates isolation by fostering shared understanding and collective moral repair.
A key component of trauma-informed care is its emphasis on creating environments that validate moral pain without judgment. This validation is particularly effective when paired with peer-led interventions, as demonstrated by the Moral Engagement Group (MEG). MEG’s structured narrative-sharing sessions enable participants to externalize guilt and shame, reframing these emotions as shared human experiences rather than personal failings. A 2023 pilot study involving 40 veterans reported a 30% reduction in depressive symptoms and a significant increase in self-compassion following 10 weeks of MEG participation.
However, the efficacy of this model is contingent on contextual factors [24], such as cultural alignment and facilitator training. For instance, peer support groups in military contexts often require facilitators with lived experience to establish credibility and trust. Conversely, in civilian settings, the absence of shared professional backgrounds may necessitate additional rapport-building measures, potentially delaying therapeutic progress.
"The integration of moral repair into trauma-informed regimes acknowledges the real human cost of moral dissonance and underpins lasting recovery."
— Dr. Jonathan Shay, Clinical Psychiatrist and Moral Injury Expert
By combining trauma-informed principles with the relational depth of peer support, this approach not only addresses the psychological aftermath of moral injury but also facilitates the reconstruction of ethical identity [10], [19], a cornerstone of sustainable recovery.
Real-World Implications and Emerging Trends
The recognition of moral injury as a distinct psychological construct has catalyzed its application across diverse professional domains, revealing implications that extend far beyond military contexts. For instance, a 2023 study by the Canadian Urological Association found that 45% of healthcare workers experiencing moral injury reported significant declines in professional efficacy [17], [25], underscoring the systemic impact of unresolved ethical dissonance. This finding highlights the necessity of addressing moral injury not only as an individual affliction but as a broader organizational challenge.
Emerging trends also point to the integration of moral injury frameworks into leadership training. The Five Eyes Mental Health Research and Innovation Collaborative, for example [18], [26], has advocated for embedding moral injury prevention into military and emergency response leadership curricula. This approach emphasizes anticipatory strategies, such as ethical decision-making simulations, which aim to mitigate the psychological toll of morally injurious events before they occur.
A critical yet underexplored dimension involves the intersection of moral injury with hegemonic masculinity. Research suggests that societal norms discouraging vulnerability exacerbate the internalization of guilt and shame [27], creating barriers to recovery. Addressing this requires interventions that deconstruct harmful gender norms while fostering moral repair, a dual focus that remains underutilized in current therapeutic models.
In conclusion, the evolving understanding of moral injury demands a paradigm shift that integrates systemic, cultural, and individual dimensions, ensuring interventions are both comprehensive and contextually adaptive.
Moral Injury Beyond the Military: First Responders and Relational Contexts
Moral injury among first responders often arises from the cumulative strain of ethically ambiguous decisions made under extreme time pressure. Unlike episodic trauma, this form of injury manifests as a gradual erosion of ethical identity, deeply intertwined with professional and relational dynamics. For example, a 2024 study published in Psychological Services found that 62% of paramedics reported persistent guilt linked to decisions about resource allocation during mass casualty events, highlighting the moral weight of their roles. This erosion is further exacerbated by organizational cultures that valorize stoicism, discouraging emotional expression and leaving moral dissonance unaddressed.
Relational contexts amplify these challenges. Family members and close peers often bear the collateral impact of moral injury, as affected individuals withdraw emotionally or exhibit self-punishing behaviors. A qualitative analysis of UK emergency responders during the COVID-19 pandemic revealed that fractured interpersonal trust and diminished empathy were common outcomes, particularly when responders internalized blame for perceived ethical failures. These relational ruptures not only hinder personal recovery but also perpetuate cycles of isolation.
To address these complexities, interventions must extend beyond individual therapy to include relational repair mechanisms. Peer-led narrative sharing [29], for instance [26], [28], has shown promise in normalizing vulnerability and redistributing moral responsibility. As Dr. Esther Murray, a leading researcher in moral injury, notes, "Healing from moral injury requires rebuilding trust—not just within oneself, but within the relationships that sustain us."
By integrating trauma-informed care with relational frameworks, practitioners can more effectively address the multifaceted nature of moral injury, fostering both individual and collective recovery.
Future Directions: Gender-Sensitive Interventions and Broader Recognition
The integration of gender-sensitive frameworks into moral injury interventions necessitates a nuanced understanding of how masculine norms intersect with trauma recovery [30], [10]. A critical aspect involves addressing the pervasive influence of hegemonic masculinity, which often stigmatizes vulnerability and emotional expression. This dynamic is particularly evident in male-dominated professions, where traditional trauma models fail to account for the moral dissonance and identity fragmentation central to moral injury. Consequently, interventions must prioritize moral repair and identity reconstruction over symptom-focused approaches.
One promising methodology is the use of narrative-based identity reconstruction, which enables individuals to reframe their experiences within a context of shared humanity and ethical growth. For instance, the Living Peace program, implemented in post-conflict settings, has demonstrated measurable success in fostering self-forgiveness and relational repair by integrating culturally sensitive storytelling techniques. A 2023 evaluation of this program reported a 40% reduction in self-condemnation scores among participants [19], [13], underscoring its efficacy in addressing moral injury through a gendered lens.
However, the effectiveness of such interventions is contingent on contextual factors, including cultural alignment and the timing of therapeutic engagement. As Dr. Esther Murray emphasizes, "Cultural sensitivity is not an optional add-on but a foundational element in addressing moral injury effectively." This insight highlights the necessity of tailoring interventions to the lived realities of diverse populations, ensuring that therapeutic models resonate with individual and collective identities.
Ultimately, broader recognition of moral injury within policy and organizational frameworks is imperative. By embedding gender-specific strategies into systemic structures, stakeholders can bridge the gap between theoretical constructs and tangible outcomes, fostering sustainable recovery pathways.
FAQ
What are the key differences between moral injury and PTSD in male populations?
Moral injury and PTSD differ fundamentally in their origins and psychological mechanisms. PTSD arises from fear-based responses to life-threatening events, engaging the threat-response system [31], [32], while moral injury stems from perceived ethical transgressions, leading to guilt, shame, and identity disruption. Unlike PTSD, moral injury often involves a profound internal conflict tied to deeply held moral beliefs. In male populations, societal norms around stoicism exacerbate moral injury by discouraging emotional expression, fostering isolation [7], [2]. Additionally, PTSD symptoms like hyperarousal and flashbacks are less central to moral injury, which instead manifests through existential distress and self-condemnation [33], requiring distinct therapeutic approaches focused on moral repair.
How do societal norms around masculinity influence the experience of moral injury in men?
Societal norms around masculinity, emphasizing stoicism, emotional control, and resilience, significantly shape how men experience moral injury. These norms discourage vulnerability [11], [13], leading men to suppress guilt and shame, key components of moral injury. The expectation to "be strong" often results in emotional isolation and maladaptive coping mechanisms, such as substance abuse or aggression. Furthermore, traditional masculine ideals, like honor and duty, intensify the internal conflict when ethical transgressions occur. This dynamic not only amplifies the psychological toll but also creates barriers to seeking help, necessitating interventions that challenge harmful gender norms while fostering emotional expression and moral repair.
What are the most effective therapeutic approaches for addressing moral injury in male veterans?
Effective therapeutic approaches for addressing moral injury in male veterans integrate trauma-informed care with moral repair strategies [27], [30]. Adaptive Disclosure Therapy (ADT) and Acceptance and Commitment Therapy (ACT) have shown promise by addressing guilt, shame, and existential distress. Peer-led interventions, such as the Moral Engagement Group (MEG), foster shared understanding and reduce isolation. Narrative-based therapies help veterans reframe experiences within ethical growth contexts, promoting self-forgiveness [19]. Additionally, spiritually integrated treatments, involving chaplains or faith-based support, address the moral and existential dimensions [10], [18]. Tailored approaches that consider military culture and masculine norms are essential for fostering long-term recovery and identity reconstruction.
How does moral injury impact male mental health in non-military professions such as healthcare and law enforcement?
Moral injury in non-military professions like healthcare and law enforcement profoundly affects male mental health by triggering guilt, shame, and identity disruption [19], [10]. Ethical dilemmas [26], [34], such as resource allocation in healthcare or use-of-force decisions in policing, often conflict with deeply held values, leading to emotional distress. Societal expectations of stoicism in these professions exacerbate isolation and discourage help-seeking. Symptoms include depression, anxiety, and burnout, with long-term impacts on professional efficacy and personal relationships [35]. Addressing these challenges requires interventions that integrate moral repair, peer support, and culturally sensitive approaches, fostering emotional expression and resilience while mitigating the psychological toll of ethical conflicts.
What role does identity reconstruction play in the recovery process for men experiencing moral injury?
Identity reconstruction is central to recovering from moral injury, as it addresses the profound disruption in self-perception caused by ethical transgressions. For men, whose identities are often tied to societal norms of honor and duty, moral injury challenges their core values, leading to self-condemnation and existential distress. Therapeutic approaches like narrative therapy and value-based cognitive-behavioral therapy (V-CBT) help men reframe their experiences [17], fostering self-forgiveness and moral repair [30], [2]. By reconstructing a coherent sense of self aligned with revised ethical frameworks, men can restore their self-worth, rebuild relationships, and achieve long-term psychological resilience, essential for meaningful recovery.
References
Frontiers | Toward a dual process model of moral injury and traumatic illness. Retrieved from https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2022.883338/full
Frontiers | Moral injury: understanding Swedish veterans who are assessed but not diagnosed with PTSD. Retrieved from https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2023.1200869/full
(PDF) Are Moral Injury and PTSD Distinct Syndromes?: Conceptual Differences and Clinical Implications. Retrieved from https://www.researchgate.net/publication/337168245_Are_Moral_Injury_and_PTSD_Distinct_Syndromes_Conceptual_Differences_and_Clinical_Implications
Moral Injury. Retrieved from https://www.ptsd.va.gov/publications/rq_docs/V33N1.pdf
Toward a dual process model of moral injury and traumatic illness - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC9448886/
Moral Injury and PTSD: Often Co-Occurring Yet Mechanistically Different | Request PDF. Retrieved from https://www.researchgate.net/publication/332601314_Moral_Injury_and_PTSD_Often_Co-Occurring_Yet_Mechanistically_Different
What are the differences between moral injury and PTSD? - Quora. Retrieved from https://www.quora.com/What-are-the-differences-between-moral-injury-and-PTSD
Title: “Navigating the Terrain: Understanding the Distinction Between PTSD and Moral Injury” – The National Association of Certified Military Chaplains. Retrieved from https://nacmc.org/2023/12/29/ptsdandmoralinjury/
Frontiers | Moral trauma, moral distress, moral injury, and moral injury disorder: definitions and assessments. Retrieved from https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2025.1422441/full
Understanding the Impact and Treatment of Moral Injury Among Military Service Members | Focus. Retrieved from https://psychiatryonline.org/doi/10.1176/appi.focus.20170023
View of Between Moral Injury and Moral Agency: Exploring Treatment for Men with Histories of Military Sexual Trauma | Medicine Anthropology Theory. Retrieved from https://www.medanthrotheory.org/mat/article/view/6876/12332
Impact of Moral Injury for Ethnic/Racial Minority Male Veterans. Retrieved from https://repository.usfca.edu/cgi/viewcontent.cgi?article=1544&context=diss
https://www.equimundo.org/wp-content/uploads/2022/06/211029_BLS21375_PRO_MasculineNorms.v06.pdf. Retrieved from https://www.equimundo.org/wp-content/uploads/2022/06/211029_BLS21375_PRO_MasculineNorms.v06.pdf
https://arq.org/sites/default/files/2023-10/Moral%20Injury-alertering%20-%20updates.pdf. Retrieved from https://arq.org/sites/default/files/2023-10/Moral%20Injury-alertering%20-%20updates.pdf
Beyond right and wrong: A new theoretical model for understanding moral injury - ScienceDirect. Retrieved from https://www.sciencedirect.com/science/article/pii/S2468749925000717
Understanding Moral Injury From a Character Domain Perspective. Retrieved from https://kcmhr.org/pdf/2021_atuel_a.pdf
(PDF) Emerging Interventions for Moral Injury: Expanding Pathways to Moral Healing. Retrieved from https://www.researchgate.net/publication/373948792_Emerging_Interventions_for_Moral_Injury_Expanding_Pathways_to_Moral_Healing
(PDF) Veterans’ experiences of moral injury, treatment and recommendations for future support. Retrieved from https://www.researchgate.net/publication/370825195_Veterans%27_experiences_of_moral_injury_treatment_and_recommendations_for_future_support
Moral Injury and Recovery in Uniformed Professionals: Lessons From Conversations Among International Students and Experts - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC9237246/
Patterns and Challenges in Help-Seeking for Addiction among Men: A Systematic Review. Retrieved from https://www.mdpi.com/2077-0383/13/20/6086
“Male suicide and barriers to accessing professional support: a qualitative thematic analysis” | Current Psychology. Retrieved from https://link.springer.com/article/10.1007/s12144-023-05423-1
What Are The Stigmas Men Face When Going Through Trauma? - Mental Health. Retrieved from https://frameworkrecovery.com/what-are-the-stigmas-men-face-when-going-through-trauma/
https://www.ijfmr.com/papers/2025/1/35779.pdf. Retrieved from https://www.ijfmr.com/papers/2025/1/35779.pdf
Recontextualising moral injury among military veterans: An integrative theoretical review - Hollis - 2023 - Journal of Community & Applied Social Psychology - Wiley Online Library. Retrieved from https://onlinelibrary.wiley.com/doi/full/10.1002/casp.2643
Frontiers | Development of an online supportive treatment module for moral injury in military veterans and police officers. Retrieved from https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2022.890858/full
Moral Injury Among Medical Personnel and First Responders Across Different Healthcare and Emergency Response Settings: A Narrative Review. Retrieved from https://www.mdpi.com/1660-4601/22/7/1055
Development of an intervention for moral injury-related mental health difficulties in UK military veterans: a feasibility pilot study protocol - PMC. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC9629100/
Full article: In harm’s way: moral injury and the erosion of trust for emergency responders in the United Kingdom. Retrieved from https://www.tandfonline.com/doi/full/10.1080/20008066.2025.2513107
Health & Wellness: Beyond PTSD: Moral Injury in First Responders | Firehouse. Retrieved from https://www.firehouse.com/safety-health/article/21241509/health-wellness-beyond-ptsd-moral-injury-in-first-responders
Moral injury and moral repair in war veterans: A preliminary model and intervention strategy. Retrieved from https://www.ptsd.va.gov/professional/articles/article-pdf/id33165.pdf
Moral injury among U.S. combat veterans with and without PTSD and depression - ScienceDirect. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S0022395622004095
Moral injury: Meaning, examples, and role in PTSD. Retrieved from https://www.medicalnewstoday.com/articles/moral-injury
Moral Injury - an overview | ScienceDirect Topics. Retrieved from https://www.sciencedirect.com/topics/psychology/moral-injury
Moral Injury in Police Work — LEB. Retrieved from https://leb.fbi.gov/articles/featured-articles/moral-injury-in-police-work
The Toll of Protecting and Serving: Treating Concurrent Moral Injury and Posttraumatic Stress Disorder in Male Police Officers | Journal of Police and Criminal Psychology. Retrieved from https://link.springer.com/article/10.1007/s11896-025-09737-7